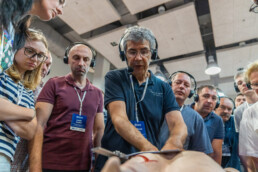
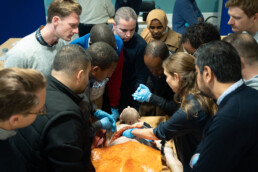
80 surgeons and anaesthetists upskilled in Kyiv, Ukraine
Our new Chief Operating Officer, Tim Law, recently returned from his first mission. Tim supported our trainers to deliver two surgical training courses in Kyiv. With logistical support from our partner World Health Organisation (WHO), 80 surgeons and anaesthetists from frontline cities learned how to treat mass trauma injuries using world-leading surgical teaching models.
To continue upskilling Ukraine’s frontline doctors, our team embarked on the challenging journey to Kyiv, first flying into Poland and travelling by bus to our final training location two days later. Despite a temporary bus breakdown in scorching heat and consequent concerns about entering Lviv before curfew, our trainers arrived safely in Kyiv and began preparing teaching materials, tools and models for the arrival of more than 80 Ukrainian doctors.
Over six days, our faculty of trainers delivered two condensed hostile environment surgical training (HEST) courses, rich in trauma surgery teachings and practical sessions.
This year, we expanded our course to include anaesthetics – a vital component of trauma surgery care. During this mission, two new faculty trainers, Dr Ian Tyrrell-Marsh and Dr Tom Dolphin, led our anaesthetics module and upskilled 22 anaesthetists from across Ukraine.

Doctors united in learning
Although united by a shared desire to manage catastrophic injuries, attendees came to our training from different Ukrainian cities.
Tim Law, our COO at the Foundation, shared: “Participation in the course was designed such that about two thirds of doctors came from front-facing oblasts or provinces. They came from Zaporizhizhia, Dnipro, Kyiv and beyond. Most of them were based in civilian hospitals.
A lot of their cities are subjected to bombardment on a reasonably regular basis. As we’re still seeing in the news, attacks lead to casualties of war, some of which are military, but many are everyday people.
Often civilian hospitals treat both civilian and military casualties, as many frontline fighters are transferred from military hospitals to make space for the next round of injured.”

Unrivalled education
Witnessing my first surgical training course in action – there is no doubt it is world-leading education.
"It was fascinating to be able to see the real value that the David Nott Foundation can add to the skills of medical professionals forced by circumstance to react to the challenges presented by armed conflict. It’s world-class education delivered by seasoned practitioners, and based on years of accumulation of course materials and conflict-specific skills.
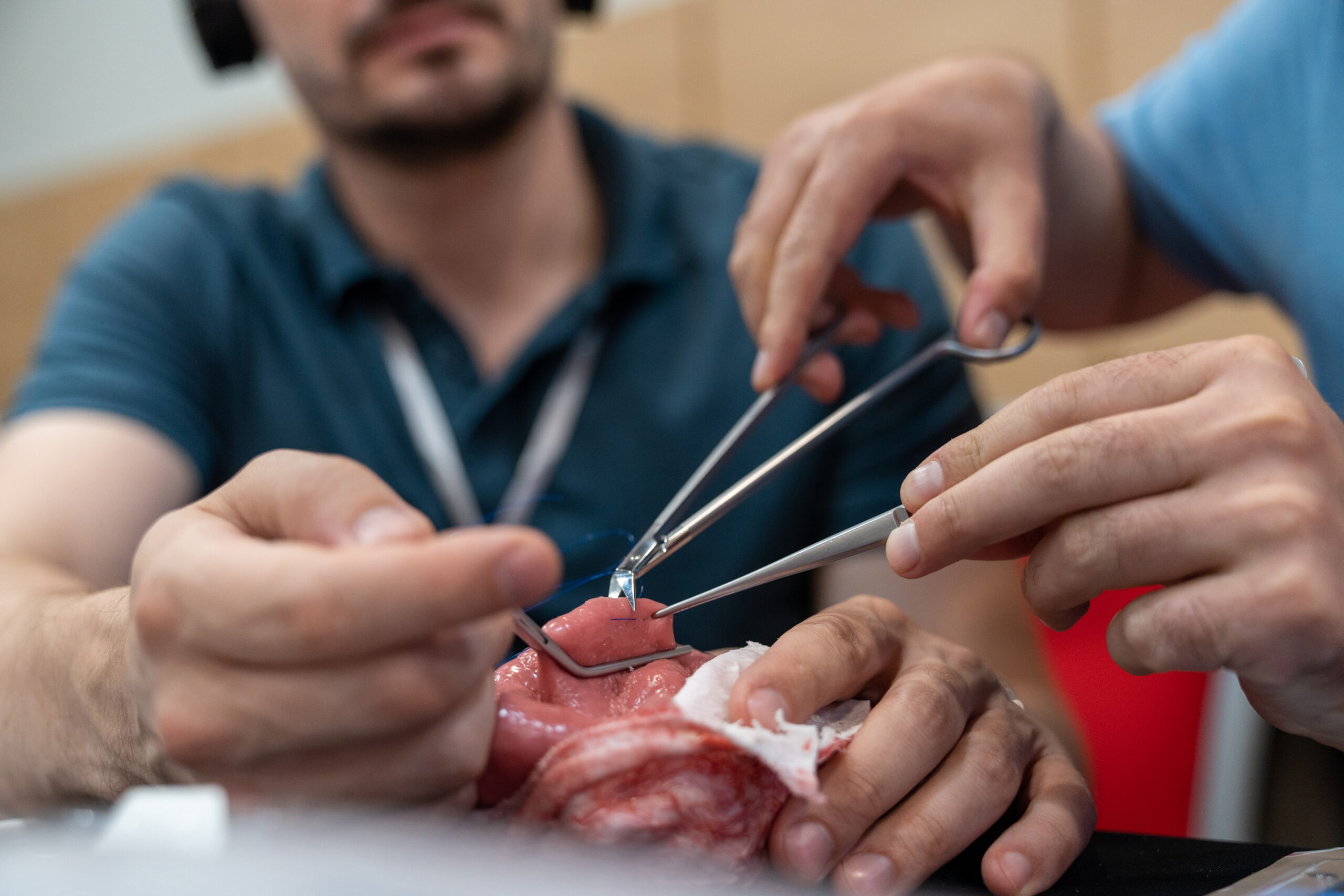
The combination of experience within the training faculty, course material quality and the practical sessions with Heston, our human body war wound simulator, enables demonstrations that otherwise aren’t possible in Ukraine,” continued Tim.
Cadavers cannot be used for teaching in Ukraine, and our war wound model has been described by surgeons as even more effective than cadaver training.
Some shared that they’ve never had access to such state-of-the-art materials and were excited to be able to take our hand-made silicone hearts back to their hospitals to continue their practice of cardiac suture repair.
Remnants of war
Although the likelihood of active conflict in Kyiv has lessened, remnants of war can be seen in and around the city. Air raids are a common backdrop, often ignored by locals as they try to continue with their everyday lives.
On the road from Lviv into Kyiv, you can see signs of Ukrainian defence. Minefield markings, skull and cross bone signs and string between trees signpost dangerous land.
On the anniversary of Ukraine’s independence, approximately 40 Russian military vehicles had been lined up along the main street. A sign that although life goes on in Kyiv, national pride and the community’s acknowledgement of their country’s continued battle remains.
“We aim to continue to develop this world-class training, such that we can continue to deliver training in the world’s most challenging environments, enabling medical professionals to enhance their skills whilst remaining close to where they are most needed", shared Tim.
"We will develop our offering to include new modules on hospital management and surgical nursing and are in the process of building a second synthetic full-body simulator and of increasing the scale of our teaching faculty. Taken together, this should enable us to increase the scale, scope and quality of our future interventions. Thank you to our supporters for helping to make these dreams a reality.”
Apply for our new Programmes Officer role
Job Title: Programmes Officer at the David Nott Foundation
Summary: This role will support the planning, delivery, and evaluation of overseas Hostile Environment Surgical Training (HEST) courses and to lead on administration for train-the-trainer and Humanitarian Sector Surgical Training (HSST) courses run within the UK. The role holder will be the lead officer for managing the supply chain for programme activity, maintaining an inventory of training materials, developing equipment manifests, procuring items in short supply, liaising with logistics contractors for international movements, and accounting for items on a routine basis. The programmes officer will also provide staff and administrative support to a range of other initiatives within the Foundation, as required. This could include helping to plan and deliver events for staff and volunteers, maintaining volunteer databases, supporting office administration, and helping fundraising and communications functions.
Accountability: Initially, this role will be accountable to the Chief Operating Officer.
The David Nott Foundation is a UK registered charity which trains doctors in the surgical skills they need to be able to provide relief and assistance in areas affected by conflict and catastrophe worldwide.
Responsibilities:
Programme Development
- Assist in the planning of overseas Hostile Environment Surgical Training missions and help lead the planning and pre-course administration of the UK-based Humanitarian Sector Surgical Training and Train the Trainer courses.
- Manage the Foundation’s HEST course training equipment including procurement, management and repair.
- Manage course logistics including booking of venues, travel bookings, security planning, visa and passport applications, elucidating vaccination requirements, and preparation/shipment/customs clearance of training materials. Assist in any other pre-course preparation required by programme managers.
- Support post-training evaluation for all courses to include student feedback and end of mission
reports.
Programme Delivery
- Deploy to high-risk countries, occasionally at short notice, to help administer course delivery.
- Provide direct administrative support to the course director for all UK-based courses.
Fundraising
- Input donor data into the Donorfy customer relationship management tool in support of the Fundraising Manager.
- Draft and dispatch thank you letters to donors and supporters.
- Dispatch merchandise and fundraising packs to supporters.
Communications
- Design and schedule social media content in support of the Head of Communications.
- Manage the enquiries inbox ([email protected]) and telephone.
- Draft, for approval, a monthly communications/programmes update email.
- Draft a monthly David Nott Foundation supporter newsletter.
- Upload news stories to the Foundation’s website.
Administration
- Support the executive team in monitoring the progress of key projects and initiatives.
- Work with the Finance Manager to keep track of invoices and payments for teaching equipment and other course expenditures.
- Manage office administration, e.g., booking of taxis, purchase of office supplies etc.
Other administrative tasks as required.
Person Specification
Over and above anything else, we are interested in providing an opportunity to someone from the London Borough of Hammersmith and Fulham who wishes to enter the humanitarian sector and who has not had the benefit of privilege in their upbringing. Desirable qualifications, skills, attributes, and experience might include:
- Knowledge of, and keen interest in, public health, current affairs, the humanitarian sector, and
international relations. - Ability, personal resilience, and willingness to travel to high-risk countries to facilitate HEST
training, which – as things stand – involves approximately 7 weeks of international and 2 weeks
of national travel per year. - Willingness to travel outside of normal office hours.
- Proven ability to manage own workload, organising and prioritising tasks to meet deadlines.
- Good communication, interpersonal and writing skills.
- An ability to manage time-sensitive work in a fast-paced environment.
- Excellent organisational skills with an ability to establish tools for effective workload
management. - Willingness to grow with the role.
In common with all staff, the role holder will need to commit to:
- Acting with honesty and integrity at all times.
- Demonstrating respect for others through consideration and empathy in all communications with colleagues and external stakeholders.
- Making an active contribution to developing the Foundation.
- Being receptive to feedback, learning from experience and others, and sharing experience and knowledge.
- Keeping others informed of issues which they need to be aware of because of their role and
responsibilities. - Consciously reviewing mistakes and successes to improve performance.
- Using discretion and being aware of issues requiring confidentiality.
The role holder must have the right to live and work in the UK, and they must not have any
restrictions on their international travel through dual nationality or an entry ban in any country
within which the Foundation might, in future, operate.
Salary: £26000-£28000, depending on skills, attributes, and experience, plus an annual personal development fund of £2000 and membership of a workplace pension scheme.
Contract Length: Permanent, with an initial probationary period of three months.
Application Details: To apply, please send a copy of your CV and a cover letter (no longer than 2 pages) stating why you want this opportunity and detailing how you meet the person specification above. State if you live in the London Borough of Hammersmith and Fulham, and whether you were a recipient of free school meals. This information will remain confidential. Please send all applications to [email protected] quoting ‘Programmes Officer’ in the subject line.
Application deadline: Midnight 29 September 2023
As attacks intensify in Ukraine, our commitment remains
Russia has intensified attacks in northeast Ukraine, prompting the Ukrainian Government to evacuate 37 settlements with the aim of preserving civilian life. A missile strike hit Chernihiv, reportedly killing seven people and injuring hundreds. As conflict and its effects continue to impact the country, a critical need for our Hostile Environment Surgical Training (HEST) remains.
Since Russia’s invasion in February 2022, we’ve trained over 250 frontline doctors from multiple cities including Odesa, Kharkiv, Dnipro, Lviv, Zhytomyr and Zaporizhzhia. We’ve also recently expanded our course to include anaesthetics – a vital component in every operating theatre.

Piecing communities back together
As offensive strikes intensify, traumatic injuries continue to increase, overwhelming hospitals’ emergency and surgical departments.
Despite teaching a significant number of Ukrainian doctors to treat patients in need of trauma surgery, hundreds still require training in skills that will help them better manage chaotic emergency rooms, surgically treat multi-organ damage and ultimately, patient by patient, piece their communities back together.

“Dozens of wounded are arriving, daily”
Our Co-Founder David Nott’s phone continues to burn with patient cases and messages from Ukrainian doctors he’s trained this past 18 months. Igor, a junior doctor from Ukraine who joined one of our courses in 2022, puts his training into practice every day. He wrote to David to share what he sees on the frontline and how his surgical knowledge is impacting lives.
Hello David,
I decided to write to you, my dear friend.
We are on the offensive. Dozens of wounded are arriving daily – both civilian and military.
There are many interesting cases - vascular injuries, abdominal trauma, many amputations. Someday, I'll put my experiences together in a film.
The doppler (a tool for monitoring blood flow) and ultrasound equipment you sent me have helped a lot.
I examine almost all injuries of the limbs with a doppler now. And of course, I use the Nott knot too (to stitch injuries).
With gratitude and respect,
Igor
Our CEO and Co-Founder, Elly Nott, said:
"Whilst the fog of war prevents us from having a precise picture of how successful Ukraine’s counter-offensive is proving, one thing we have a clear view of at the David Nott Foundation is the fortitude and dedication of Ukraine’s war doctors.
As Igor’s letter states, Russian attacks do not spare civilians - in fact they target civilian infrastructure - and dozens of wounded are arriving daily in hospitals like his. Health facilities are not immune from Russian targeting, with Physicians for Human Rights reporting that 1014 attacks have been perpetrated against Ukraine’s hospitals, health workers, and other medical infrastructure since February 2022.
The fight for Ukraine’s freedom continues and we will keep sharing knowledge and providing support as long as we are needed.”
Help us train more of Ukraine's doctors
This World Humanitarian Day
This World Humanitarian Day, we reflect on our commitment to the humanitarian values that inspire our work - training medical professionals to provide safe, skilled surgical care in countries impacted by conflict and catastrophe.
Our flagship Hostile Environment Surgical Training (HEST) course continues to provide the best in surgical training to those who need it most. Using innovative teaching materials such as our prosthetic hearts, kidneys, arteries and veins, our world-class trauma surgery modules are brought to life by the remarkable, talented training faculty who deliver it. We are so grateful to our team of trainers who give up their time to share knowledge with doctors around the world. We know they also learn as much from them in return.
In addition to training surgeons, we have developed an anaesthesia module, expanding our focus from the surgeon to the wider - any equally important - operating theatre team. As with surgery, conflict presents unique challenges for anaesthetic practice including severe blast injuries, blood loss and resource constraints.
I was inspired to start our Foundation by a single, grainy photograph of David.
In a room in a hospital in Aleppo, lit solely by the steady beam of a projector, he was discussing cases with a group of Syrian doctors at the end of a day of operating. I started thinking how that life-saving training delivered by David in Aleppo, built on decades of frontline experience, could be brought to hundreds, perhaps thousands, more doctors.
David’s unwavering connection with the doctors of northwest Syria goes back a decade and when the devastating earthquake hit southern Türkiye and northwest Syria in February, we immediately started discussing with local partners and colleagues what they were seeing and how we could help. It rapidly became clear that thousands of survivors were left with life-altering injuries in need of surgical treatment and rehabilitative care.
Thanks to expert navigation of local permissions by our partners, we were able to run a joint teaching and operating mission with Action for Humanity in Aqrabat Hospital, Idlib. The Action for Humanity team saw 300 patients in clinic before completing 60 surgeries the following week. Above the operating theatres, we equipped 35 Syrian doctors with the surgical techniques they need to treat complex injuries inflicted by the earthquake or ongoing conflict.
Ninety percent of our training faculty on the mission were Syrian and based in the northwest, therefore able to better understand local health system challenges and teach the course in Arabic.
Sustainability is vitally important to us; we want surgical knowledge to be embedded in communities to the extent that it is self-perpetuating and we are no longer needed. Until it is, we’ll keep returning as long as we are needed, No Matter What.
As a small charity, we are able to deliver so much more in terms of training and value for our donors’ money by partnering with other humanitarian organisations like Action for Humanity. Our training partners are diverse in scale and size. We delivered training in Moldova with the World Health Organisation and for Yemeni surgeons with Médecins Sans Frontières. We are excited to collaborate with MedGlobal in the coming months, and in Ukraine, were proud to partner with our friends at UOSSM, a charity initially formed to provide relief and assistance to Syrian civilians affected by the deadly conflict there.
Unfortunately, risks for humanitarians and attacks on healthcare have increased in recent years.
Last week, Physicians for Human Rights reported that 1014 attacks have been perpetrated against Ukraine’s hospitals, health workers, and other medical infrastructure since February 2022. Recent Elrha research also revealed that attacks on Syrian health facilities have deterred people from accessing health services and seeking help when needed.
Every hospital bombed, every healthcare worker killed, denies people vital care and destabilises communities both physically and psychologically. These atrocities are under-reported and we are honoured to support the campaigning efforts of Action for Sama, seeking to raise awareness of and ensure accountability for attacks on healthcare.
We believe in safe, skilled surgical care for all and stand with the communities we serve, No Matter What.
Elly Nott, Co-Founder and CEO
‘Keep Calm and Channel On’
A team of four recently formed a relay and swam the English Channel to raise funds for four different charities. Kate Ribeiro dos Santos swam the first relay leg, raising an outstanding £5540 for our cause. Here, Kate shares her experience and how the team kept each other motivated through the night.
We started at 11.41pm from Samphire Hoe, near Folkstone.
I started the relay which was probably the most surreal swim of my life - jumping into the sea in the middle of the night with a couple of flashing lights on my head and costume!

The first few hours in the dark were very gritty, mainly due to sea sickness but also the cold and lack of sleep.
Two of the team were very ill, despite having taken all the medication we could have taken, and it took incredible metal strength for them in the water. We saw that another relay failed after 4 hours due to sea sickness. However, once the sun came up, the sea became calmer, we doubled up on the medication and things got a lot more enjoyable!

We saw loads of cargo ships and ferries, as well as 10 other Channel teams out in the Channel with us. I had an amazing 3rd swim covering nearly 7km due to the current and we made great time.
The reason for the slightly long route of the swim is due to tides and currents. Only super fast swimmers can go straight across, the rest of us need to take more of an 'S' shape. Finally, Ness brought us in to France with an epic last swim and we finished at 2.41pm UK time.
What a day and what an incredible team! I'm not sure I have ever done an event which relies more on teamwork than this.
If anyone had stopped or got out, we would have had to turn back. Everyone is equal and has to pull their own weight - literally!
I have smashed the target I never thought I would have reached in the first place - £5,540! I hope the Foundation are as happy as I am!
Dr Esayas Mustefa - Becoming the calm in any storm
Dr Esayas Mustefa is the only general surgeon within a 130km radius in Ethiopia. When we trained him during one of our UK HEST courses, we knew we’d come across a very talented surgeon who would make an outstanding trainer. We’ve since upskilled Esayas to become a David Nott Foundation trainer, upskilling his peers. Here, he shares the impact of his new skills in the Afar region of Ethiopia.
Since my first training with the Foundation in December 2021, the war has been a bit calmer in Afar. There have been a few leftover soldiers, but it is calmer. Nonetheless, with the energy and resource invested in us, many patients have been helped because of my training.
Controlling bullet damage
I remember a patient with a bullet to the right of his groin. That day, I remember I was home. The emergency surgeon didn’t call me and did a laparotomy, but then decided he needed me to come in when he saw the damage.
There was an extensive haematoma (build up of blood) in the pelvis. I thought it was a vascular injury but didn’t have the proper instruments or stitches to fix it.
That’s when I did damage control.
I got proximal and distal control of the bleeding, which I learned on the course. I managed to dissect the haematoma and with the help of the other surgeon, I did a bypass. This means putting in a tube conduit that bypasses the dissection, allowing blood to carry on flowing through the vessels as normal.
We transfused him with blood and transferred him to specialist care, to have his vascular surgery. It was great.
Passing on life-saving skills
I’m also really, really happy to share what I’ve learned on the course. We have two emergency surgeons and I do my best to teach them.
They didn’t know how to do colectomies, resections, anastomoses, or some basic decision making in difficult times. I’ve taught them these things, and also when to operate and when not to operate.
Now they know to ask me – they call to ask me questions. We have a good working relationship.
The difference between life and death
I’m now also confident with abdominal injuries. I’m a better surgeon, and those I teach are better, because of the training I had with David.
Explosive injuries, I was never used to. I usually see bullets. Even seeing photos of explosive injuries used to get to me. But seeing David’s live videos in training stimulated me to be ready for anything.
Calm in a storm
In all honesty, no matter how many patients I saw or the injuries I faced – bullets, road traffic accidents – every time I opened an abdomen, I used to get nervous. No matter how much I’m used to these patients, I don’t know how to describe it. The anxiety would come.
After I met David, I thought how many years will it take me to get to that level of calmness?
But with the course, I learned to be really calm and collected in demanding situations.
For me, my patients, my future patients, and those willing to learn from me - have all benefitted from my training.
More on our latest Train The Trainers course
Hospice Ukraine raises over £50,000 to better serve the terminally ill
Photo credit: Hospice Ukraine and the Royal Society of Medicine, London
As part of a special Hospice Ukraine event raising funds for palliative care in Ukraine, our Co-Founder David Nott was invited to share his reflections of upskilling over 200 Ukrainian doctors during eight missions, and the importance of fighting for continued holistic healthcare - from the beginning of life to the end - during war.
Since Russia’s violent attacks against Ukraine began last February, the Ukrainian people’s access to healthcare has suffered immensely. We know conflict leads to reduced medical equipment, medicines, specialist care and hospital staff numbers. Despite our mission focussing on saving lives with skilled surgery, palliative care for the terminally ill remains of equal and vital importance.

Hospice Ukraine is a charity that believes everyone deserves access to high-quality palliative care, no matter where they live. But the upheaval of war has overwhelmed the ability of Ukrainian healthcare professionals to support those nearing the end of life.
To better provide comfort, dignity and care for the terminally ill, Emily Maitlis and Jon Sopel came together at the Royal Society of Medicine in London to host a special fundraiser organised by palliative care doctor, writer and Co-Founder of Hospice Ukraine, Dr Rachel Clarke.
When asked how David copes working in war zones like Ukraine, he shared: "Humans become incredibly resilient under pressure. It's what we train (during our courses too). We're not going to waver, we'll be here for our friends in Ukraine until this war is over."
David was joined by fellow speakers such as writer and comedian, Adam Kay, and world-renowned former neurosurgeon, Dr Henry Marsh, who holds deep connections with doctors and academics in Ukraine. Guests also heard a selection of beautiful songs from a Ukrainian refugee choir now based in the UK.
Speaking of the remarkable ability for the terminally ill to exude love and concern for others as they near death, Adam Kay shared, "The thing I realize (during a 2-hour conversation with a patient) is that none of her many concerns are about herself; it's all about the kids, her husband, her sister, her friends. Maybe that's the definition of a good person."

A live auction, which included a piece of work donated by Grayson Perry, led to a final fundraising figure of £50,000. We will continue to advocate for healthcare excellence and the people of Ukraine, for as long as this war wages on.
“Seeing Syria again, despite its sadness, there’s still a sense of pride”
Dr Ammar Darwish has been part of the Foundation’s family for over a decade. Ammar volunteered as a trauma surgeon in Aleppo when Syria, his home country, was oppressed and targeted by the Assad Regime. There, he met our Co-Founder David, forming a brotherhood like no other. Here, Ammar shares how it felt to return to Syria to lead our earthquake surgical mission.
Faculty Lead: Dr Ammar Darwish. Faculty Trainers: Dr Pete Mathew, Dr Mahmoud Hariri
When I heard that an earthquake had struck northwest Syria and Türkiye, I was in Ukraine training doctors on the frontline of the Russian war. Colleagues from Syria were frantically calling loved ones seeking news. I knew then that we needed to find a way to reach the affected Syrians, as Syria’s already weakened healthcare system would buckle under further strain.
After the earthquake, it became clearer how essential it was that we reach Syria.
Thousands left with unattended injuries
We immediately started to receive reports from the ground that survivors were facing complex trauma wounds in huge numbers. Crush wounds, large, open injuries, serious infections that have led to the need for amputation. As we expected, there was and remains an enormous need for surgical training and support.
There was also a need for psychological support – hope, confidence, and to know that they are not alone.
Unfortunately, it took about a week before international aid entered northwest Syria to help victims. There were thousands of casualties and to have this delay, in an already crumbling healthcare system due to 12 years of war, was a disaster within a disaster for the Syrian people.
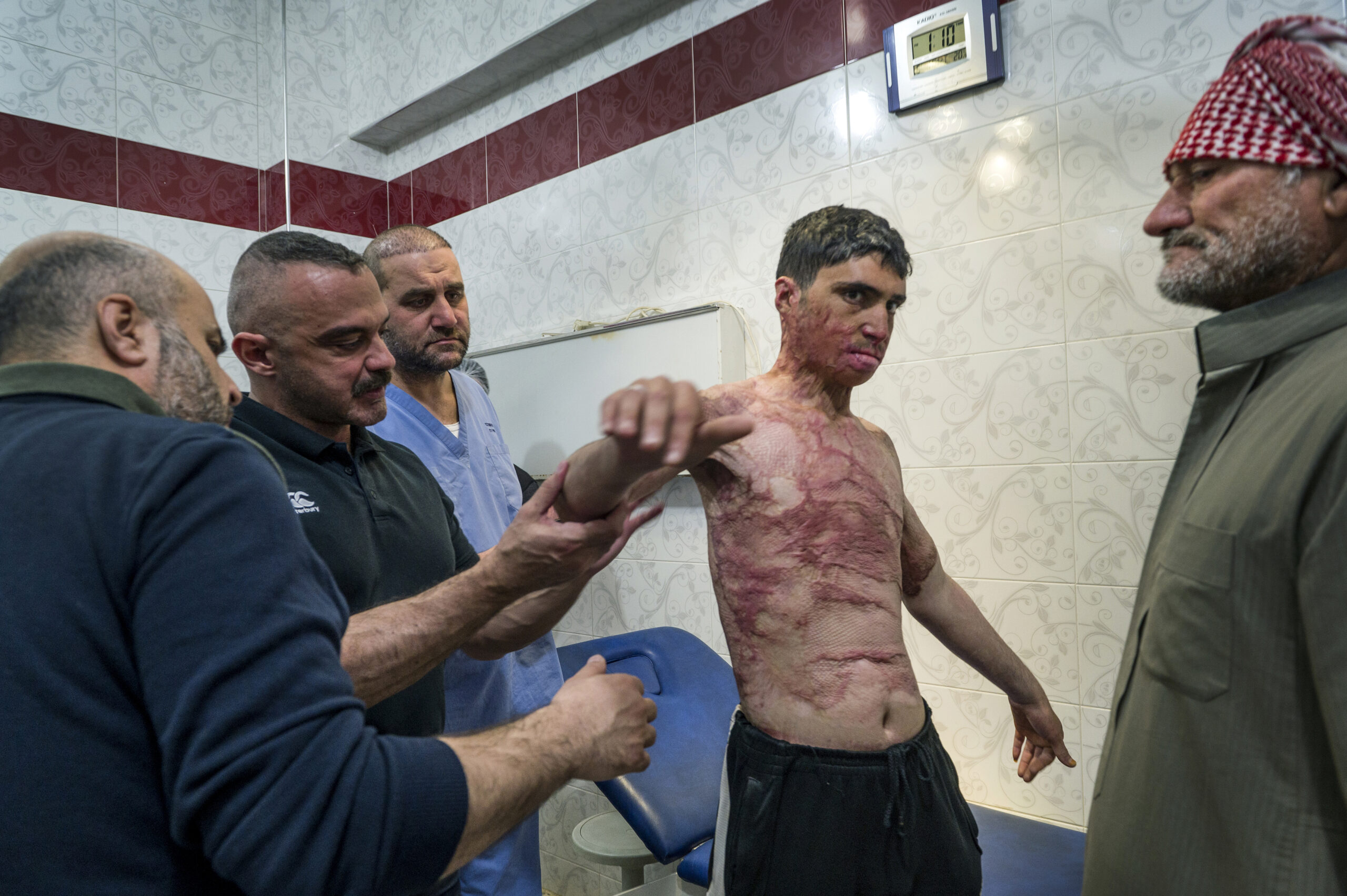
This devastating delay and the lack of equipment, medical supplies and resources meant that more people were suffering with severe injuries left untreated and many developed further complications as a result.
After humanitarian organisations were granted entry, we joined forces with Action for Humanity, formally Syria Relief, to plan a mission like no other. We wanted to use our time as effectively as possible, achieving as much as we could during a week-period.
Maximum impact
We delivered our world-class hostile environment surgical training (HEST) course in Arabic to local surgeons. We used our cutting-edge, one-of-a-kind teaching equipment, including our human wound simulator model, Heston, and printed vessels, kidneys, hearts and bowel, to arm them with skills for treating complex wounds.
This was our first course whereby 90% of it was delivered by local Syrian training faculty - surgeons we had trained during the conflict that started in 2011. It was a proud moment for the Foundation.

Feedback has been wonderful and encouraging – that our training is very important, their skills have improved, and they wished they’d had this training before.
We also upskilled and empowered 9 of the surgeons to become surgical trainers themselves so they could share their new, advanced skills with peers in their hospitals. They were very excited. We had approximately 23 trainees who received our HEST course, included newly qualified surgeons and other specialised surgeons from 9 hospitals in northwest Syria.
Action for Humanity worked all hours to get us safely into the country. They were outstanding and very well informed. It shows preparedness is really important for a smooth mission. They also led the operating side of our joint mission, performing surgeries on about 80 patients, including children, over 7 days. An exceptional feat, treating severe injuries from both the war and earthquake.
Proud to be home
Physically entering Syria was something else. Going back to Syria was a remarkably moving day for me. Crossing the border, seeing Syria again, with all the sadness and atrocities that have happened, there remains a sense of pride. It was a very special feeling.
Meeting the doctors and seeing those we’ve worked shoulder to shoulder with and trained before was very moving. Reunited after years, yet our bond remains the same. Even those who had not met David were asking about him – they are so keen to learn from him. It was a very, very emotional moment.

Welcomed with open arms
The Aqrabat Hospital, where we delivered our training, was fantastic. They changed the whole setting of the hospital to accommodate us and our course.
On the day we left, the hospital held an Arada for us, which is a typical Syrian parade and song to show us their gratitude for the work that has been done. Leaving Syria was quite emotional for everyone.
The need for surgery, training and support continues. The earthquake has put Syria back under the spotlight – and this time I hope it reminds in the public’s minds. We must work to restore Syria to its former glory, before the ravages of conflict and collapse.
We’ll be back to do our part.
Join our team as Programmes Manager
Job title: Programmes Manager
Summary: This role will be responsible for the planning and execution of overseas and
UK-delivered Hostile Environment Surgical Training (HEST) courses including
all related logistics. The Programmes Manager will be the key person
responsible for maintaining day-to-day relationships with operational
partners on-the-ground and liaising with HEST course leaders. They will also
be principal point of contact with our Training Faculty, highly committed and
experienced senior medical professionals who volunteer their time and skills
to deliver HEST. This role will carry additional functions including managing
and developing online teaching resources and events and ensuring the supply
and delivery of David Nott Foundation (DNF) surgical models.
The David Nott Foundation is a UK registered charity which trains doctors in
the surgical skills they need to be able to provide relief and assistance in areas
affected by conflict and catastrophe worldwide.
Accountability: This role will managed by and accountable to the Chief Operating Officer.
Responsibilities
Responsibilities include, but are not limited to the following:
Programme Delivery
- Support the executive team in the delivery of all training activities, both in the UK and overseas.
This will include management of logistics, travel and risk management in close collaboration
with our operational partners in-country. It will also include preparation of the courses ahead of
time and attendance at each course to ensure that they run smoothly. - Manage the logistical planning and deployment of the HEST Faculty when they run the HEST
courses internationally. Be their primary point of contact for all missions and respond to any
enquiries that they may have. - Manage the planning and delivery of all training activities, both in the UK and overseas,
including:- Identification and prioritisation of high-impact locations and training audiences.
Building of preparedness to enable a quick and effective response to new and emerging
crises. - Identification and management of potential course locations to judge the suitability of
venues, partners and delegates both in the UK and overseas. - Liaison with key partners and facilitators such as the World Health Organisation (WHO),
Médecins Sans Frontières (MSF) and Action for Humanity. - Management of course logistics including booking of venues, travel bookings, security
planning, visa advice, elucidating vaccination requirements, and shipment of training
materials. - Point of liaison for the training Faculty, including managing their availability and
providing support functions such as risk management ahead of trainings. - Working with the Head of Communications and Engagement to respond to enquiries
from the media and relevant media content from courses. - Managing post-training evaluation for all courses to include student feedback and end
of mission reports. - Responsibility for all the DNF’s HEST course training equipment including procurement,
management, and repair. - Management and organisation of Webinar Series including liaison with Faculty and participating
doctors to organise cases for discussion.
- Identification and prioritisation of high-impact locations and training audiences.
Administration
- Support in monitoring the progress of key projects and initiatives.
- Maintain contact lists and databases such as Donorfy.
- Identify, evaluate, report, and mitigate risk associated with the planning and delivery of
programmes. - Assist in the management of any interns working on the Programmes at the Foundation.
- Work with the Finance Manager to keep track of invoices and payments for teaching equipment
and other course expenditures. - Management of contracts with training venues and partner organisations.
- Other administrative tasks as required.
Person Specification
- A degree in a relevant subject or equivalent professional experience.
- A good knowledge of, and keen interest in, public health, current affairs and international
relations. - Ability, personal resilience, and willingness to travel to high-risk countries to facilitate HEST
training, which – as things stand – involves approximately 7 weeks of international and 2 weeks
of national travel per year. Including travel outside of normal office hours. - Proven experience of contributing to overseas projects, trainings, or events, particularly in high-risk countries.
- Proven experience of risk management and mitigation strategies.
- Proven ability to manage own workload, organising and prioritising tasks to meet deadlines.
- Excellent communication, interpersonal and writing skills.
- The ability to manage time-sensitive work in a fast-paced environment.
- A natural diplomat, with proven ability to establish and maintain effective working relationships
in a multicultural and multidisciplinary environment, together with the ability to communicate
and negotiate at all levels. - Excellent organisational skills with proven ability to establish tools for effective workload
management. - Willingness to grow with the role.
All staff will commit to:
- Act with honesty and integrity at all times.
- Demonstrate respect for others through consideration and empathy in all communications with
colleagues and external stakeholders. - Make an active contribution to developing the Foundation.
- Be receptive to feedback, learn from experience and others and share experience and
knowledge. - Keep others informed of issues which they need to be aware of because of their role and
responsibilities. - Consciously review mistakes and successes to improve performance.
- Use discretion and be aware of issues requiring confidentiality.
Salary: £40-45,000 per annum, based on experience.
Contract Length: Permanent, with a probationary period of six months.
Closing Date: Monday 3 July 2023.
Application Details: To apply, please send a copy of your CV and a cover letter (no longer than 2
pages) detailing how you meet the person specification above. Please send all applications to
[email protected] quoting ‘Programmes Manager’ in the subject line.