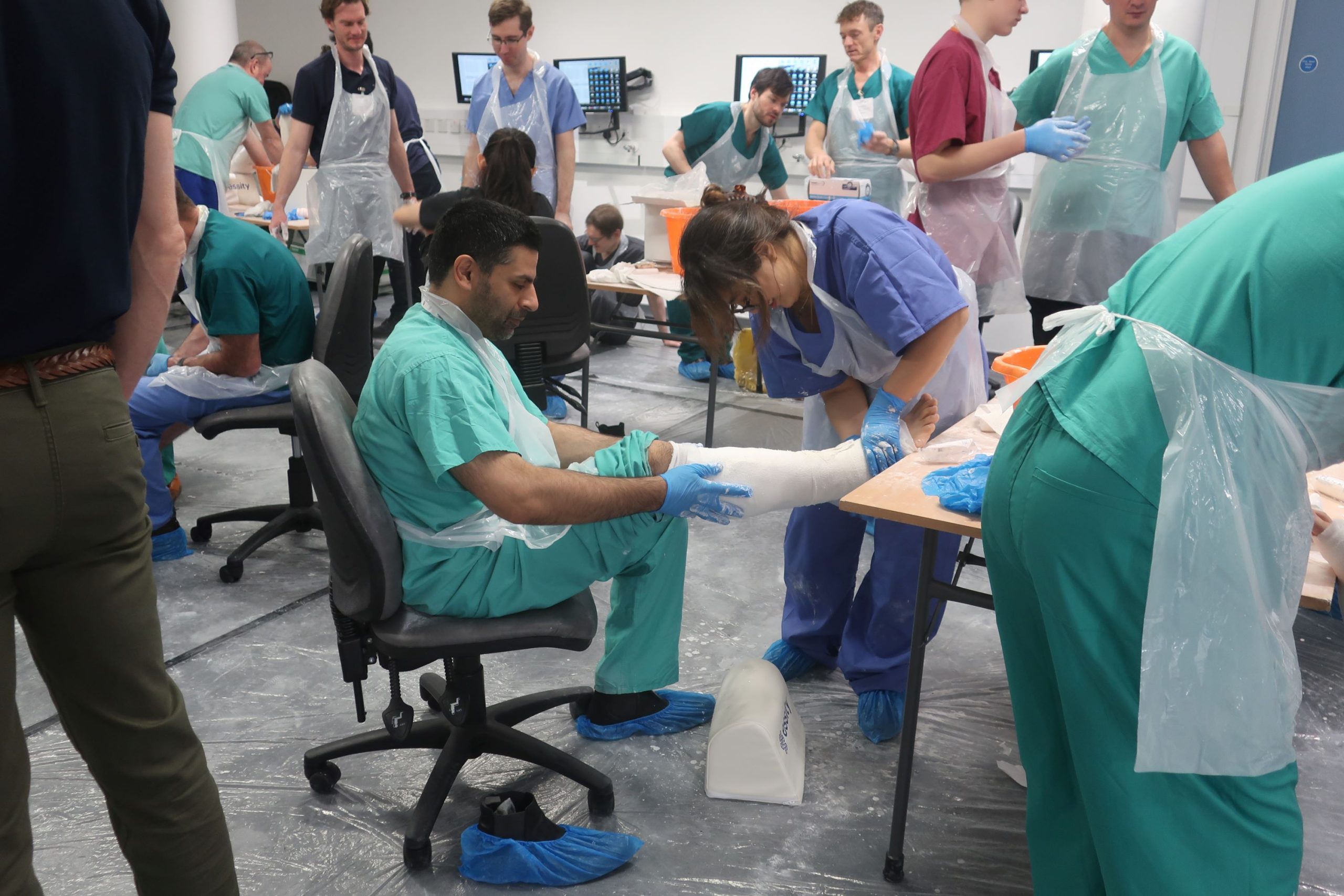
Strengthening global surgical capacity through HEST-UK training
Building on the success of our partnership with the Royal College of Surgeons of Edinburgh (RCSEd) in June, where 24 surgeons were equipped with vital skills to save lives and limbs in conflict zones, we joined forces again this December to train an additional 23 surgeons. Our trauma surgery training in the UK (HEST-UK) aligns with RCSEd's broader mission to support global healthcare by equipping professionals to address healthcare needs in low-resource or conflict-affected areas.
Designed for medical professionals working in, or preparing to travel to, conflict and disaster zones, our HEST-UK course brought together participants from around the world. Surgeons traveled from as far as Hong Kong, New Zealand, Australia, Ukraine, and the USA to take part in this transformative week of intensive training.
The course provides comprehensive training in surgical techniques for managing injuries frequently encountered in conflict zones, such as blast and shrapnel wounds, with a dedicated focus on Obstetrics and Gynaecology during the final day. Regardless of their specialty, surgeons gain the skills needed to handle complex trauma cases and significantly improve patient outcomes.
This immersive training integrates real-life trauma case presentations from conflict zones like Syria, teaching models designed specifically for our programmes, and hands-on practice using human cadavers, delivering an unparalleled learning experience.

A Global Effort
The David Nott Foundation and the Royal College of Surgeons of Edinburgh are charitable organisations, and our work is made possible by the generous support of donors and sponsors. We are deeply grateful to The Russell Trust, Essity, BBRAUN, Stryker, and BMA Giving for their invaluable provision of equipment and consumables, which enabled us to deliver this course.
BMA Giving generously granted £10,000 to cover the costs of specimens and equipment for this training. Given the nature of this project, there was significant interest from individuals working with NGOs and other non-profit organizations, where high course fees often present a barrier to accessing training. Thanks to the support of BMA Giving, we were able to reduce fees, ensuring the course was more accessible to a broader range of participants.
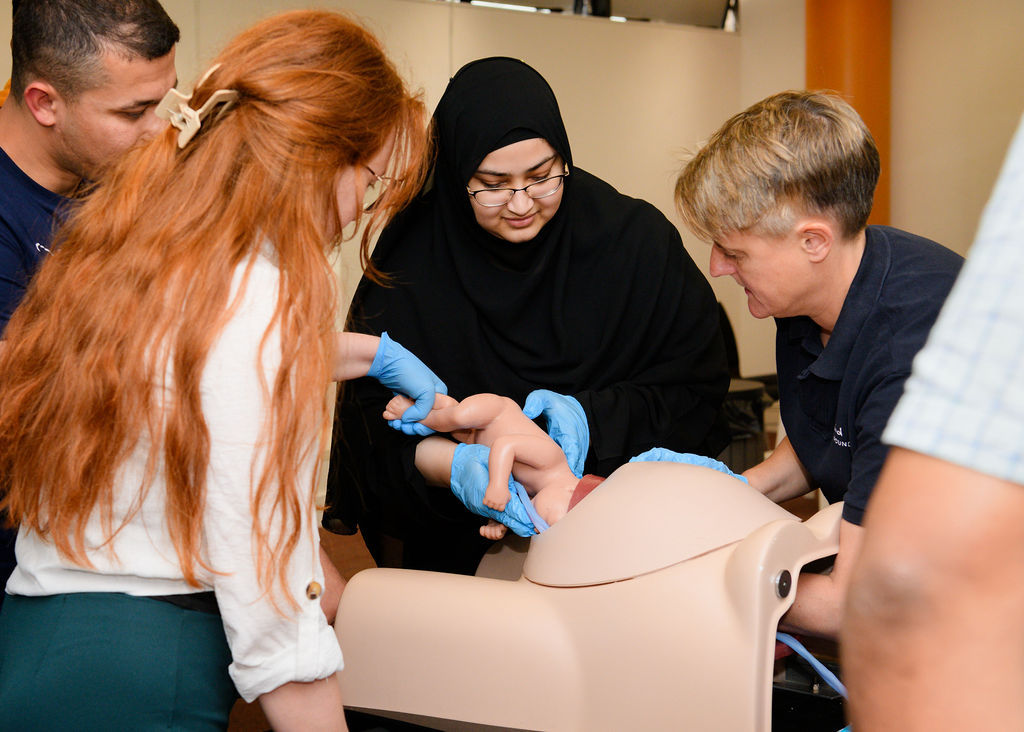
Empowering Ukrainian Surgeons to Save Lives
As part of our 2024 localisation efforts in Ukraine, we sponsored three Ukrainian doctors who had previously completed our trauma training courses to attend our Hostile Environment Surgical Training (HEST-UK). This advanced training provided a unique opportunity for them to refine their skills further by practicing on cadavers. They also received dedicated mentorship from our expert faculty, including David Nott, who shared insights drawn from over 30 years of trauma surgery experience in conflict zones.
Upon returning to Ukraine, these doctors joined our growing local Ukrainian faculty to train more surgeons on the ground during this difficult period. Their newly acquired skills were put to immediate use, with reports of life-saving interventions within days of their return.
"Just two days ago, I faced a mass casualty incident involving four patients in one hour. Three of them suffered massive hemorrhages from arterial injuries, fractures, and amputations. I was the only surgeon available. The skills and knowledge I gained through the courses offered by the David Nott Foundation saved their lives and their limbs." - Dr Volodymyr H, Ukrainian General Surgeon
Our most recent training in Ukraine
24 doctors trained during 1st UK course with Royal College of Surgeons Edinburgh
For the first time in partnership with Royal College of Surgeons of Edinburgh (RCSEd), we delivered a Hostile Environment Surgical Training UK (HEST-UK) course to equip 24 surgeons from across the globe with vital skills needed to save lives in conflict and disaster zones.
Aimed at medical professionals who work in, or are planning to travel to, conflict and catastrophe zones around the world, our HEST-UK course brought together surgeons from across the globe, including Australia, Poland, Finland, Denmark, Libya and six from Ukraine, for a transformative week of intensive training.
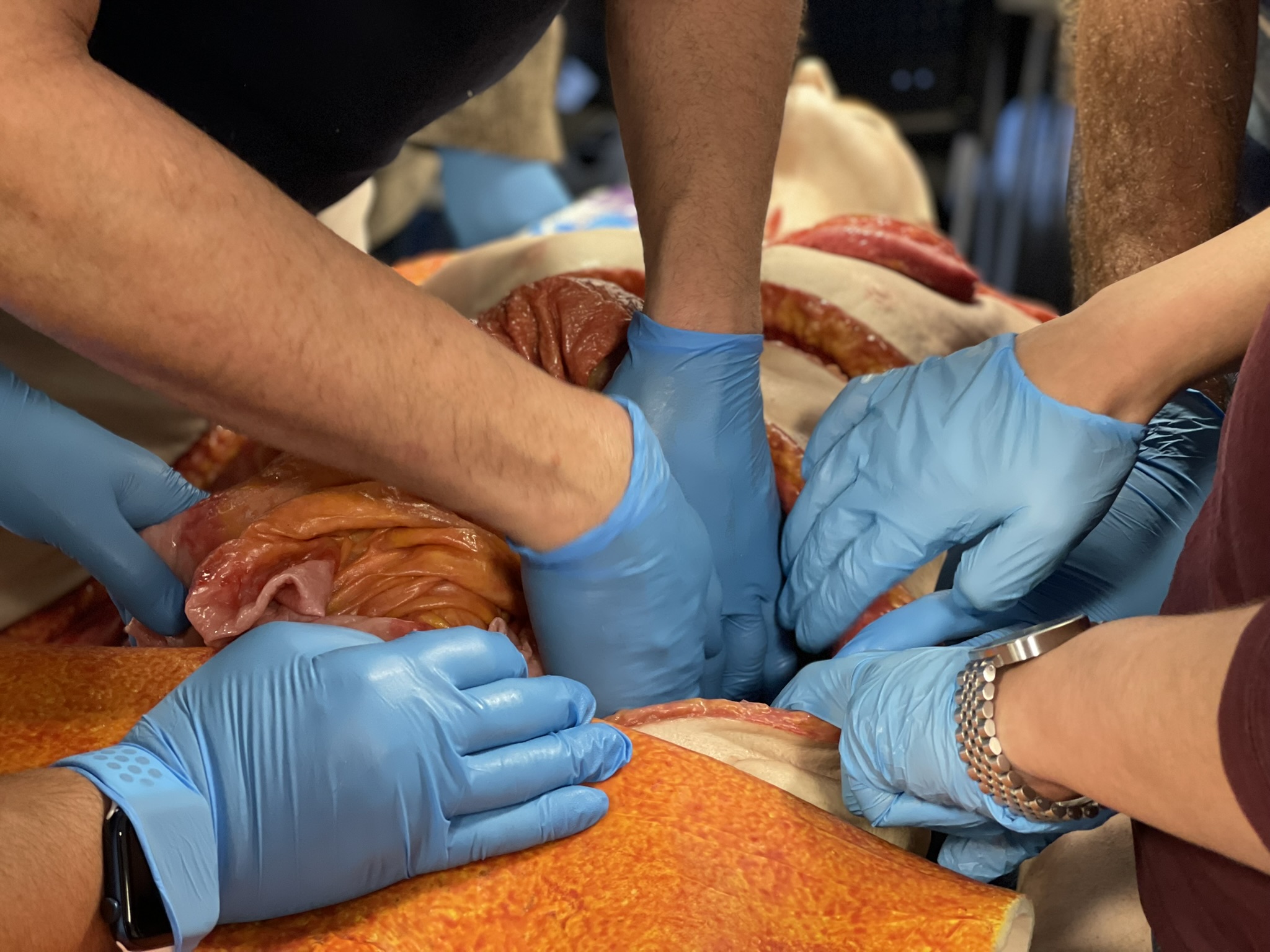
This marks the beginning of our brand-new partnership with RCSEd, joining forces to upskill humanitarian surgeons and frontline trainers in the making. Our course combined trauma case presentations taken straight from war zones like in Syria, our cutting-edge teaching models designed especially for our use, and human cadavers.
Dr Igor Belkin, HEST-UK participant and surgeon from Ukraine who we sponsored to join our training, said:
“The course was great! All frontline methods were described in detail in theory, and then with the help of DNF trainers, we then worked on and learned more about using cadavers.
These skills are always useful, especially in a country that is at war. After completing another DNF course in Zaporizhizhia in February 2023, I used many learnings in field surgery. Now in Edinburgh, I got even more practice with cadavers.”
Dr Senka Stojanovic, HEST-UK participant and general surgeon from Poland, said:
"Now, possibly more than ever during our lifetimes, the world is fraught with problems of growing divisions and inequality, which among other things impacts access to quality healthcare, affecting not only the current generation, but future ones as well.
I felt incredibly fortunate and grateful for the opportunity to learn first-hand from some of the leading experts in the field.
"The wealth of experience and practical tips brought by the faculty was unmatched and cannot be found in textbooks or surgical atlases."
I highly recommend this unique course to any surgeons who plan to or already work in humanitarian settings around the globe, but who need to build on their confidence and skill to provide surgical care outside of their surgical specialties."
Mariette Naud-Betteridge, Director of Partnerships and Stakeholder Engagement at RCSEd, said:
“Witnessing the course first-hand revealed the extensive practice and diverse disciplines required to deliver surgical care in conflict zones. Not only did the course’s structure and the dedication of David and his faculty bring challenging cases to life, the delegates' intense focus and eagerness to learn emphasised the course’s relevance and necessity.
Collaboration between the David Nott Foundation and RCSEd demonstrates our shared commitment to equipping medical professionals with the critical skills and confidence needed to save lives in the most demanding situations. Special thanks also to all who supported the course, including sponsors B. Braun, Essity, and Stryker. RCSEd look forward to welcoming back the DNF team and a new set of delegates in December for the next HEST-UK Course.”
As fighting intensifies across Ukraine, Palestine, Sudan and beyond, there has never been a greater need for skilled, humanitarian surgeons around the world. That’s why our programme of bespoke training courses are so vital and we will continue to grow our international network of war doctors.
Sign up to our next HEST-UK course
“If this training can work in Gaza, it can work anywhere else.”
Dr Israar Ul-Haq joined our HEST-UK (Hostile Environment Surgical Training-UK) course in Bolton to improve his trauma surgery skills before entering the heart of Palestine’s crisis – the Gaza Strip.
Dr Israar Ul-Haq is a doctor with a primary focus on urgent and pre-hospital care. Volunteering his expertise, Dr Ul-Haq joined two separate missions to Gaza, serving in Khan Younis and Deir al Balah.
“As I entered Gaza I felt a mix of emotions—eager to employ the skills I learned from HEST and help those in need, yet wary of the drones I can hear as soon as I entered.”
With minimal resources and an overwhelming patient load, ranging from 500 to 1000 individuals daily according to Dr Ul-Haq, the medical staff faced immense challenges. The injuries they treated ranged from blast injuries and crush wounds, to traumatic amputations and fatal head injuries, or gun shot and sniper wounds. Techniques learned during the HEST course, such as medical triage or procedures for getting access to the chest quickly, such as thoracotomies, were immediately put into action.
It impacted every aspect of my work in Gaza
Dr Ul-Haq shared: “The course impacted every aspect of my work in Gaza, such as understanding the local environment and the types of injuries we encountered. Whether it was performing chest drains, managing blast injuries, conducting debridement, or treating burns, the training equipped me with the necessary skills I needed.
The lectures on burns were very useful, they directly influenced our treatment protocols. Techniques like thoracotomy and bleeding control learned during the course became standard procedures in our daily practice. The emphasis on conducting primary and secondary surveys, along with fast scanning helped us to quickly assess and address critical issues in a high-pressure setting."
Patients that stay with us
“One patient's case is stuck in my head. He presented with a shrapnel injury to his back, which had penetrated his thorax. While we stabilised him initially, signs of Beck's triad (low blood pressure, distended neck veins, and distant or muffled heart sounds) alerted us to a possible cardiac tamponade (a serious condition where fluid builds up around the heart) - I had learned to identify this issue through fast scanning during the course. We rushed him to the operating theatre. Employing techniques like the clamp shell procedure, we successfully removed the bleeding around his heart, stabilising him.”
“We had a four-year-old brought into the hospital with a pneumothorax, severe head injuries, and burns. We immediately admitted the child to the ICU. We performed a chest drain to treat the pneumothorax and employing rapid sequence induction (a method to quickly administer anaesthesia and secure the airway) to stabilise the child's condition. We debrided the wounds at the back and used fluid therapy to manage shock and maintain stability.”

Our course is not just about building medical skills, it's about cultivating problem-solving abilities in the most challenging of circumstances. In environments where resources, staffing, and traumas are at their peak, the course empowers doctors to think laterally and use whatever limited resources they have. From using different pain management drugs to conducting fast scans to evaluate a patient's condition rapidly, every aspect of the training is geared towards equipping doctors with the tools they need to save lives, no matter where they are.
“Upon arrival, another patient had no bleeding or shrapnel injuries, but vitals would not stabilise. drawing on what we learned from the HEST course, we identified a left-sided pneumothorax. Despite initial stabilization efforts, the patient's vital signs remained unstable,” shared Dr Ul-Haq. “I often used the fast-scanning technique taught in the course. ; I detected an additional right-sided pneumothorax. Without hesitation, I proceeded to insert a chest tube, a procedure ingrained in our training. Had we delayed any longer, the outcome could have been disastrous.”
“Gaza is facing unimaginable suffering, and HEST was incredibly helpful there. If it can work in Gaza, it can work anywhere else too.”