“Maternal health - it's a societal barometer.”
Every two minutes, a woman loses her life to preventable causes related to pregnancy and childbirth. These staggering statistics stress the need for action. In humanitarian crises, where access to healthcare is severely limited, maternal care becomes even more critical.
“800 preventable maternal mortalities are happening every day, and a woman dies every two minutes from a preventable cause. So that's women dying through pregnancy and pregnancy related conditions,” shared Dr Pippa Letchworth, our Faculty Lead for Obstetrics and Gynaecology.”
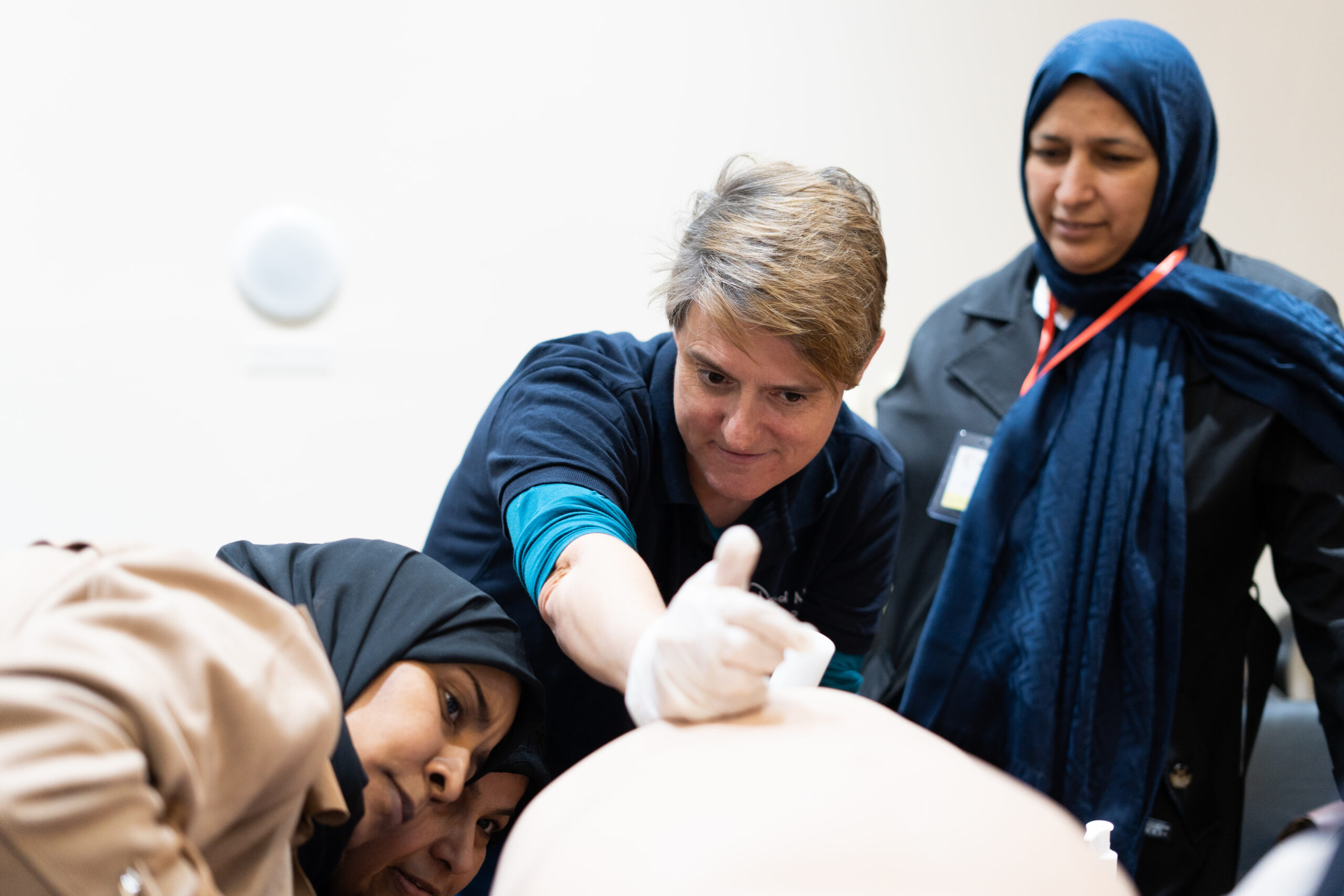
This sobering reality is what drives our passionate team to develop an obstetrics and gynaecology course aimed at addressing the most pressing challenges in maternal healthcare. In crisis settings, where resources are scarce, the course equips healthcare professionals with the skills needed to perform life-saving surgeries, particularly focusing on addressing the top global killers of women - haemorrhage, obstructed labour, sepsis, and unsafe abortion.
“75% of displaced people are women and children, and one of the five of those women will be pregnant.”
The course covers a wide spectrum of topics in maternal and neonatal healthcare in crisis. Participants begin with trauma training before transitioning into obstetrics to understand the complexities of childbirth emergencies.
Emphasis is placed on neonatal resuscitation techniques with the goal of reducing the number of stillbirths. Subsequent sessions address postpartum haemorrhage management, perineal repair, and navigating challenging deliveries like impaction and breech positions. The course also covers disruptive delivery, crucial for situations where doctors have limited access to caesarean sections.

Beyond the medical realm, our trainers advocate for a holistic approach to maternal health in their teaching. It's not just about reducing mortality rates, it's about understanding the wider implications of maternal deaths on families, communities, and societies at large. Children left motherless are at a significantly higher risk of mortality and developmental issues, perpetuating a cycle of vulnerability.
“There needs to be a call to arms to improving maternal health.”
We must advocate for women's rights, improving doctors access to education and dismantling systemic barriers that perpetuate maternal mortality.
DONATE
103 surgical life savers in Tripoli, Libya
We’re back from a week in the Libyan city of Tripoli after completing a first-in-our-history mission. We upskilled 103 doctors – the largest number trained on one mission – and trialled our brand-new obstetrics and gynaecology course.
Libya’s history is marked by political turmoil and civil unrest. The uprising against the rule of Gaddafi led to brutal violence against Libyan civilians and instability across the country. Today, 13 years after the ruler’s death, conflict between armed groups continues and Libya’s security remains fragile.
Outside of politics, Libya has been devastated by natural disaster. In September of 2023, heavy rain caused the collapse of two dams, leading to horrific damage and the loss of thousands of lives. Wounds inflicted by violence or natural disasters often require rapid surgical care, with a need to focus on controlling the worst of the damage first.

Surgical toolkit for any crisis
In a bid to empower Libyan doctors with skills to treat wounds caused by war or natural disaster, we partnered with the Libyan Board of Medical Specialties to deliver four surgical training courses in parallel. Over five intense days, our team of expert trainers delivered two trauma surgery courses, two anaesthesia courses and a brand-new obstetrics and gynaecology course.
According to a 2023 UN agency report, a woman dies from pregnancy or childbirth every two minutes. During conflict, women are less likely to seek maternal care and hospitals are under-staffed or under-resourced. That's why our trainers created a bespoke obstetrics and gynaecology course to help doctors better protect mothers and their babies in war and catastrophe.
During the week, we trained 103 doctors. Doctors we’d previously upskilled in Libya also joined our training faculty and led the teaching of a number of our modules for the first time. Dr Aisha Alghamji was one of them.

It really was paralysing
Dr Alghamji shared: “I remember I have a case of a 70-year-old lady. We found there was a huge bleed in her tummy. Most of her blood is – in minutes – almost drained out. It really was paralysing – what to do? She doesn’t have that much time.
"That lack of knowledge paralysed me. She is a living, human being – with dreams, hopes, a whole community. She is part of it. It keeps haunting you, that feeling. What I could do differently?"
She lost her life.
After 2018 when I attended the course with the Foundation, there is something shifted in my way of thinking. It did that thing for me, that confidence the surgeon needs to do more than their best – to run the extra mile for the patient.

I faced another case similar to it (this lady). I told immediately to me brain – ‘damage control! Damage control!’. I was able to send her home. She is alive, she is a grandmother, she is everything.”
A resilient healthcare system
Dr Moez Zeiton, Consultant Orthopaedic Surgeon and our Faculty Lead for Libya, said: “It is a privilege to have had the opportunity to lead the single most ambitious series of courses for the foundation, training over 100 doctors in a week. It was a huge effort from the foundation’s team and superb faculty to get over the line.
Candidates in Libya travelled from every part of the country with many travelling over 1000km to participate in our surgical training. Their eagerness to learn and share their own experiences was evident and they will now be equipped with the skills needed to deliver high quality care to their patients. "
This marks the beginning of continued training in Libya and a commitment to gifting doctors with extensive trauma skills to handle any challenge.
HELP US FUND MISSIONS IN LIBYA
War Doctor Heroes: Meet Dr Aisha
War Doctor Heroes features the stories of our global family of surgeons. Their devotion to saving lives inspires us to keep moving forward. Conflict doesn't stop, neither do we.
In this feature, we're proud to introduce Dr Aisha from Libya. Dr Aisha travelled 1,000 miles to attend our HEST course in Misrata, Libya. She is part of a small team of surgeons in Sabha, south west Libya. She is used to fighting to keep patients alive whilst shrapnel and bullets tear through her hospital building. “A single shot to an oxygen tube could have destroyed the whole theatre, where we were operating but we couldn’t stop – we felt we were making a difference”. After our course, Aisha said: “Your hands can do the work but you need someone to guide you”.
Help us train more war doctors like Aisha by donating here https://lght.ly/1jbkc1g
HEST in Libya
It was the early hours of 4 March when our DNF team touched down at Misrata airport. David and Ammar were this time joined by Harald Veen, formerly Chief Surgeon of the Red Cross and now a valued addition to our teaching faculty.
Over the next three days they taught 55 Libyan doctors in the skills they need to provide the best surgical care for patients with complex injuries.
The doctors had travelled from across the country from towns including Tripoli, Misrata, Houn and Sabha. The majority specialised in general surgery but there were also orthopaedic surgeons, an obstetrician and a neurosurgeon present; demonstrating the relevance of our training programme to all medical specialities.
 HEST faculty in Misrata
HEST faculty in Misrata

The course concluded with a practical workshop at Misrata Central Hospital where they put their newly-learnt skills into practice with tuition from David, Ammar and Harald on vascular, general surgical, neurosurgical and facio-maxillary techniques.

We have already had three applications for scholarships from surgeons attending the Misrata course and look forward to continuing to build our friendships with the doctors of Libya.