Dr Israar Ul-Haq joined our HEST-UK (Hostile Environment Surgical Training-UK) course in Bolton to improve his trauma surgery skills before entering the heart of Palestine’s crisis – the Gaza Strip.
Dr Israar Ul-Haq is a doctor with a primary focus on urgent and pre–hospital care. Volunteering his expertise, Dr Ul-Haq joined two separate missions to Gaza, serving in Khan Younis and Deir al Balah.
“As I entered Gaza I felt a mix of emotions—eager to employ the skills I learned from HEST and help those in need, yet wary of the drones I can hear as soon as I entered.”
With minimal resources and an overwhelming patient load, ranging from 500 to 1000 individuals daily according to Dr Ul-Haq, the medical staff faced immense challenges. The injuries they treated ranged from blast injuries and crush wounds, to traumatic amputations and fatal head injuries, or gun shot and sniper wounds. Techniques learned during the HEST course, such as medical triage or procedures for getting access to the chest quickly, such as thoracotomies, were immediately put into action.
“It impacted every aspect of my work in Gaza”
Dr Ul-Haq shared: “The course impacted every aspect of my work in Gaza, such as understanding the local environment and the types of injuries we encountered. Whether it was performing chest drains, managing blast injuries, conducting debridement, or treating burns, the training equipped me with the necessary skills I needed.
The lectures on burns were very useful, they directly influenced our treatment protocols. Techniques like thoracotomy and bleeding control learned during the course became standard procedures in our daily practice. The emphasis on conducting primary and secondary surveys, along with fast scanning helped us to quickly assess and address critical issues in a high-pressure setting.”
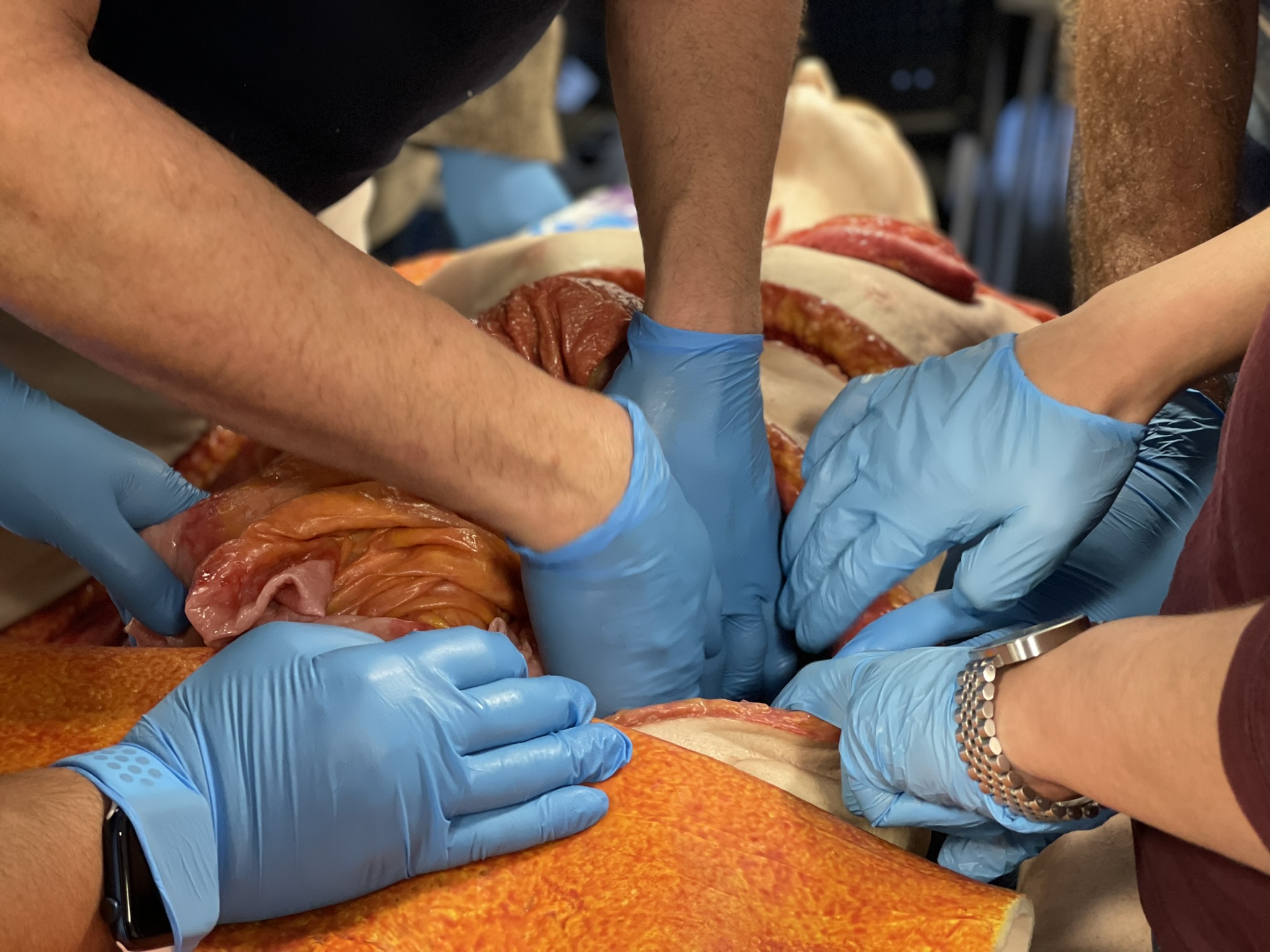
Patients that stay with us
“One patient’s case is stuck in my head. He presented with a shrapnel injury to his back, which had penetrated his thorax. While we stabilised him initially, signs of Beck’s triad (low blood pressure, distended neck veins, and distant or muffled heart sounds) alerted us to a possible cardiac tamponade (a serious condition where fluid builds up around the heart) – I had learned to identify this issue through fast scanning during the course. We rushed him to the operating theatre. Employing techniques like the clamp shell procedure, we successfully removed the bleeding around his heart, stabilising him.”
“We had a four-year-old brought into the hospital with a pneumothorax, severe head injuries, and burns. We immediately admitted the child to the ICU. We performed a chest drain to treat the pneumothorax and employing rapid sequence induction (a method to quickly administer anaesthesia and secure the airway) to stabilise the child’s condition. We debrided the wounds at the back and used fluid therapy to manage shock and maintain stability.”

Our course is not just about building medical skills, it’s about cultivating problem-solving abilities in the most challenging of circumstances. In environments where resources, staffing, and traumas are at their peak, the course empowers doctors to think laterally and use whatever limited resources they have. From using different pain management drugs to conducting fast scans to evaluate a patient’s condition rapidly, every aspect of the training is geared towards equipping doctors with the tools they need to save lives, no matter where they are.
“Upon arrival, another patient had no bleeding or shrapnel injuries, but vitals would not stabilise. drawing on what we learned from the HEST course, we identified a left-sided pneumothorax. Despite initial stabilization efforts, the patient’s vital signs remained unstable,” shared Dr Ul-Haq. “I often used the fast-scanning technique taught in the course. ; I detected an additional right-sided pneumothorax. Without hesitation, I proceeded to insert a chest tube, a procedure ingrained in our training. Had we delayed any longer, the outcome could have been disastrous.”
“Gaza is facing unimaginable suffering, and HEST was incredibly helpful there. If it can work in Gaza, it can work anywhere else too.”
