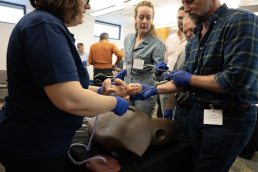
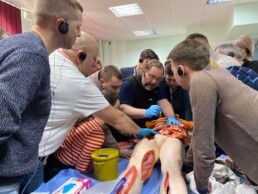
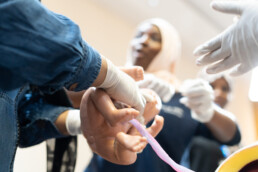
Preparing 36 Kuwaiti doctors for surgery in Gaza
With support from the Foreign Common Development Office (FCDO) and Kuwaiti Red Crescent Society (KRCS), we upskilled 24 Kuwaiti surgeons and 12 anaesthetists who intend to volunteer as humanitarians in Gaza. This marks our first direct partnership with the UK government.
Faculty Lead: Dr Ammar Darwish. Surgical Faculty: Dr Mahmoud Hariri, Professor Steven Mahoney, Dr Saladin Sawan, Dr Juan Robinson. Anaesthesia Faculty: Professor Pete Mahoney, Dr Oliver Harrison and Dr Hussein Nagi.
Kuwait is home to over 4.2 million people. Sandwiched between Iraq and Saudi Arabia, Kuwait is a small but influential country in the Middle East. As the war continues to wage in Gaza, a number of Kuwaiti doctors have plans to volunteer their skills on the frontline. Upon invitation from the FCDO and KRCS, we were pleased to upskill 36 doctors and prepare them for complex trauma injuries.
Our Co-Founder, Elly Nott, said:
“Recognised by the UN as a Humanitarian Center and embodying the values of charity and humanity, Kuwait is a natural partner for the David Nott Foundation. During this mission, we trained 24 surgeons and 12 anaesthetists in partnership with the Kuwaiti Red Crescent Society and the British Embassy, Kuwait.
The doctors have been trained in surgical skills essential for saving life and limb and will contribute to relief campaigns and humanitarian initiatives in the region. There is sadly no end of need for their skills in the world at present and we look forward to further collaboration with our colleagues here in Kuwait for the benefit of those who suffer in conflict.”
The skills required by doctors in Gaza at this time extend far beyond surgery. Being calm in a crisis, able to adjust to the needs of the patient in front of you and adapt to the hospital’s resources – or lack of - are absolutely vital. Doctors and anaesthetists that rely on innovative surgical tools or drugs will only have so much impact in active war zones.
Consultant Anaesthetist and DNF Faculty Trainer, Professor Pete Mahoney, said:
“In conflict zones, there may not be reliable electricity, water or access to medical gases such as piped or cylinder oxygen. You need to be able to pivot and use something called ‘draw-over’ anaesthesia to deliver suitable medication. This is when the use of simple masks or a bag can be used to pull volatile agents (anaesthetic medications) into the patient’s body.
We also taught the Kuwaiti doctors how a simple anaesthesia machine can be constructed from components as they may need to build one in the field with whatever the hospital has. It is critical that humanitarian doctors are able to adapt.”
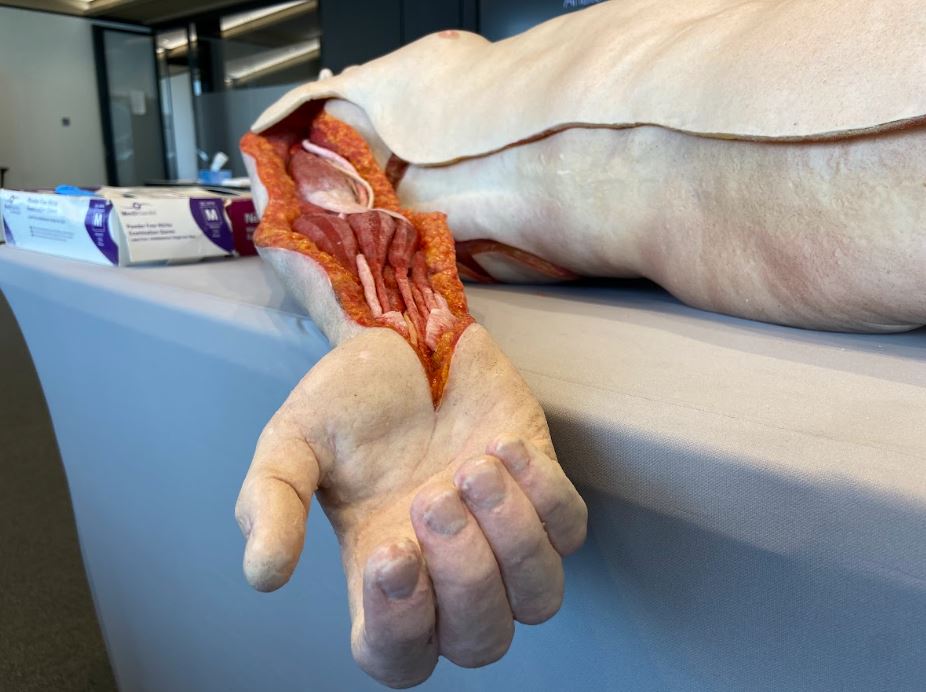
We know from our Faculty Lead in Palestine that doctors on the ground don’t always have the time or available tools to fix bones together with metal pins. To give doctors other options that require less equipment, we taught Kuwaiti doctors how to set bones with plaster casts, which can help breaks to heal in the absence of pins.
The British Ambassador to Kuwait, Mrs Belinda Lewis, said:
“The fact the UK government’s first partnership with the amazing David Nott Foundation took place in Kuwait is testament to the strong and productive relationship between our two countries. This combination of British and Kuwaiti expertise will undoubtedly support the medical response to the dreadful suffering in Gaza.
I am grateful for the assistance of a number of people in Kuwait who have helped me to bring in this expert team from the UK, and I would like to pay special thanks to Professor Ghassan Abu Sittar, veteran war surgeon and humanitarian, who first suggested this valuable partnership to me.”
President of the Kuwaiti Red Crescent Society and former Minister for Health in Kuwait, Dr Hilal Al Sayer, said:
"On behalf of the Kuwait Red Crescent Society, I extend my appreciation to the British Embassy for their facilitation of the training course throughout this process. I also extend our sincerest gratitude to the David Nott Foundation for their invaluable expertise. Their guidance has empowered our esteemed consultants with the skills needed to navigate the complexities of emergency medical care as volunteer medics in conflict zones whose dedication serves as a testament to the spirit of humanity that defines our National Society.
Last, but certainly not least, I extend my heartfelt thanks to the National Bank of Kuwait for their generous support, we are truly grateful for their partnership.
I am immensely proud of the collaboration that has characterized our time together and am confident that we will carry forward the lessons learned in our shared mission to serve humanity with compassion and expertise."

Until we can support and upskill doctors on the ground in Gaza, we will continue to do all we can from a distance. The delivery of our surgical and new anaesthesia courses to Kuwaiti doctors who intend to enter Palestine as humanitarian volunteers, forms part of our unwavering commitment to the ongoing crisis.
SUPPORT OUR TRAINING
“The patients. The families. They’re all in my head.”
Our Co-Founder David Nott recently travelled to Rafah, Gaza, to help treat the thousands suffering from war injuries, malnourishment, and everyday ailments that have progressed to life-threatening conditions because of delayed treatment. Here, David shares what he witnessed, what the urgent medical needs are on-the-ground, and how those he met are tattooed onto his mind.
After travelling from Cairo and getting closer to Gaza, it was quite a shocking experience. At the Rafah crossing, you could see miles worth of trucks in a queue trying to get in.
Driving through Gaza, it was like an enormous refugee camp with tents everywhere. Every single place that wasn't occupied by somebody had a tent on it. Most of the tents were so packed against each other it was difficult for people to walk.
"Thousands and thousands of people were in a small area. They had nowhere to go."
Treating those more likely to live
The hospital I was working in was called Al Najjar Hospital, the only semi-functioning hospital in Rafah. It was small, with a limited number of beds, but ended up housing thousands of people. Every corner was full. Patients were in the corridors, all over the wards, lying on the floor, five people where one might stand. There were people on the floor that were dying, some that had died - people crying out for help.
I had to step over people to get to patients. I had to make rapid decisions on whether or not they could be saved – decision-making techniques that we teach to those that attend our courses.
The hospital only had two operating theatres. There was no intensive care unit and no ventilators, so I had to decide which patients should be operated on with the best possible outcome. On ward rounds we reviewed those that had been treated, but many had infections because of limited sterile space or antibiotics.
18th century illnesses
"Because thousands of people have been compressed into small spaces, and many haven’t sought medical care for their everyday conditions, the clinical needs in Gaza today are astonishing."
It’s not just war wounds that doctors face – ruptured appendices, hernias, ulcers, gangrene. General surgery has been delayed for months on end and people are dying or losing limbs as a result of problems that could have been resolved quickly.
This is the reality of trauma in war – some traumas that were not traumas to begin with become life-threatening – racking up death tolls even further.
"Outside of war wounds, 21st century doctors are dealing with 18th century illnesses."
Children with chest infections were developing a condition called empyema - their infections had become so bad that their lungs were filling with pus. I’d never seen that before – it’s an 18th century condition that you would never see today.
Post-operative care felt impossible. Say you amputate somebody’s leg, there’s nowhere for them to go to recover safely. Tents aren’t sterile and it has been so cold, with the wind coming off the beach.
Calm amongst the chaos
Despite the chaos, Gazan doctors are truly outstanding. They were so warm and helpful. They were grateful that people were there to help, and together we did everything we possibly could.
This war zone is different to the others I’ve been in. The volume of people and the lack of basic medical or human resources made it incredibly challenging.
They urgently need field hospitals, more staff, a huge amount of medical resources. They need more doctors, nurses, rehabilitation services, physiotherapists. But not only that, they need a safe place for patients to go to recover after operations. Their medical aid needs are huge and doctors in the field need to be supported.
"Seeing Gaza reminds me of the vital importance of our foundation’s work. Training doctors, operating on patients in war zones, bearing witness to doctors’ needs on the ground, I’m more driven than ever to help the charity grow so we can reach even more people in need."
The patients, the families, they’re all in my head. They will always stay in my head.
SUPPORT OUR TRAINING IN PALESTINE
Bearing witness to the medical needs in Gaza
Our Medical Director Dr Ammar Darwish embarked on an operating surgical mission to Gaza to offer his trauma surgery skills to those most in need. As he crossed the border into the besieged territory, he faced trucks held up for miles, filled with much-needed aid.
“The needs in Gaza - it was hell on earth”
As Dr Darwish travelled deeper into Gaza, he observed the expanse of makeshift tents, shelters for internally displaced families. Some had no tents at all, resorting to crafting shelters from plastic sheets that offered little protection from the cold and wet weather.
Entering Khan Yunis Hospital, Dr Darwish was met with exhausted medical staff who were battling with limited supplies. Vast numbers of patients with extreme injuries came through the doors and difficult choices had to be made within minutes on who could be saved.
Adapting to an impossible environment
Lack of electricity and water are causing numerous health complications. Without electricity, patients in need of ventilation struggled to breathe. The absence of water prevented the sterilisation of medical tools. Medication, antibiotics, painkillers, and even anaesthesia were sparse – basic resources that should be present in any hospital.
Children with severe injuries from shrapnel lay in beds with little to no relief due to lack of medical resources.
“I met a very scared six-year-old boy that had a shrapnel injury in his abdomen. Because of the complexity of the injury, and because of limited resources such as antibiotics, the boy’s abdomen was open and there were a lot of holes in his bowels. Anything he ate or drank was leaking out of his abdomen. That child had not had any food to eat, or a proper drink, for a whole month, he was a skeleton.”
Stretched to limits
Despite the chaos, resilience and humanity ran through the Gazan people. Local medical staff welcomed Dr Darwish and his team, despite managing the loss or unknown status of their homes or family members. They were stretched to their limits, with only nine operating hospitals left of all the 36 hospitals in Gaza.
“You cannot but compare it to our work in a UK major trauma centre, where for one trauma patient, you might have six, seven, even 10 doctors treating them. In Gaza you are one doctor for 10 people, 15 people, which means you have to make really heavy decisions on who to treat. It sits heavy on my heart that there were many children we could not even see to in time.
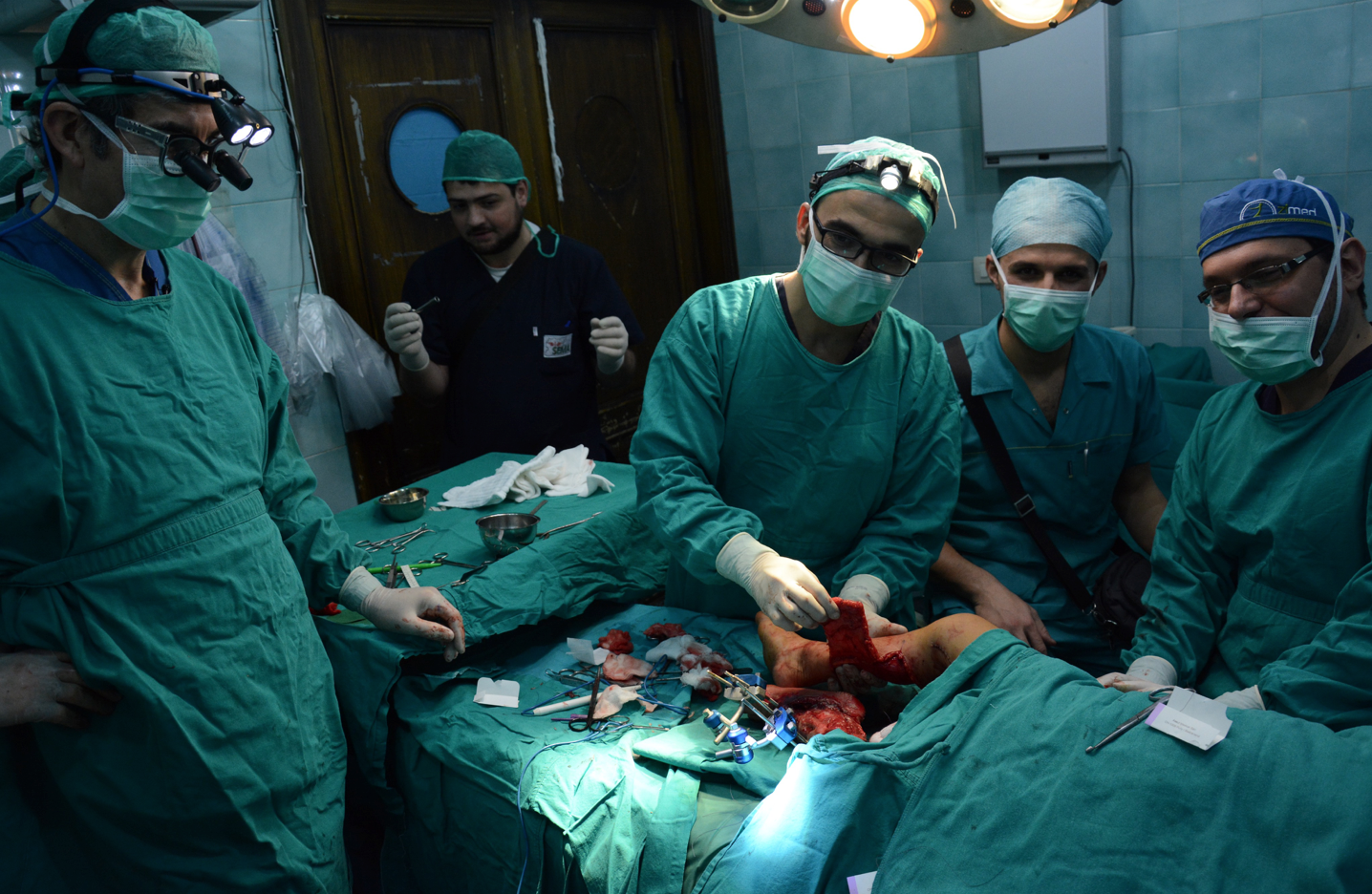
I've been part of over 45 global missions in conflict zones, with Syria, Aleppo, being one of the most challenging. This mission to Gaza was the most difficult mission that I've been through physically, mentally, even psychologically, because of the amount of injury that I witnessed and the amount of devastation and carnage we were faced with and with only basic supplies and resources.”
Medical needs for years to come
“The number of injured people now in Gaza has exceeded 70,000. If you can imagine the complexity of these injuries - these patients will need years of medical care, surgical operations, physiotherapy, and a lot of resources to reconstruct their injuries. There is a huge need for humanitarian aid, but first there must be a ceasefire.”
We have provided training to 79 UK surgeons who are preparing to or have already travelled to Gaza to provide life-saving aid. Many more are scheduled to depart. Our aim remains steadfast and unwavering – to ensure everyone has access to safe, skilled surgical care.
We are committed to supporting the Palestinian people until we are able to train in-country again.
SUPPORT OUR TRAINING IN PALESTINE
Teaching 86 war doctors in Vinnytsia, Ukraine
86 more Ukrainian doctors are now armed with trauma surgery skills that will help them improve the care they give to victims injured on the frontline. In partnership with UOSSM International, our trainers upskilled both surgeons and anaesthetists in the Ukrainian city of Vinnytsia.
Despite over two years of conflict, many doctors in Ukraine are still facing horrifying injuries - and many they were not trained to treat during standard medical training. War inflicts incomprehensible injuries on those it meets. Shrapnel can tear through multiple parts of the body and it’s a medical team’s job to identify which injury needs treating first. This is done by carrying out damage control to find and reduce sources of bleeding before repairs can take place. Under pressure, this isn’t an easy feat but are vital skills that we teach – alongside guidance on how to stay calm and focused - on our course.

The long road
It’s not just immediate care that doctors need to be trained in. War wounds often require months, sometimes years, of rehabilitation and additional surgeries. Our team visited the Superhuman Center in Vynnyky, Lviv, an outstanding facility supporting adults and children who have lost limbs in the war. It is facilities like these, and training like ours, that help doctors carry out amputations in such a way that the victims will recover well or receive prosthetics when the time comes.
Nick Cartwright, our Programmes Manager who led this course and visited facilities at both Superhuman and Unbroken, said:
“There’s a lot of a hardship in Ukraine today, but a lot of hope. There’s a strong desire for our training – Ukrainian doctors want to know they are doing absolutely everything they can for those injured in their communities. Having now upskilled nearly 600 doctors in Ukraine, the country’s healthcare systems are getting stronger, despite the ongoing pressures of war.”

Frontline stories
We interviewed a number of doctors who took our surgical and anaesthesia courses in Vinnytsia. It’s their experiences that drive us to keep going back to new cities, spreading trauma surgery knowledge further across the country.
“People were burning”
“When the war started we had a lot of humanitarian aid it was so helpful. But we still need it – the war hasn’t finished. This course is so helpful and interesting – there’s a lot of information and practical skills. Many things were new for me. It’s great that I now have new skills and knowledge.
I have some experience of war wounds since the war. We’ve had attacks here in Vinnytsia, a lot people were injured. People were burning, some had head injuries, they came to our emergency hospital. I also volunteered in places like Donbass.
The biggest attack here was on the 14th of July. A lot of people were killed, children. It was hard because we didn’t prepare for this. On this course, we saw a video of how colleagues work in an emergency situation. We have some things we need to change on how we will work in an emergency.
I want to tell the world that war in Ukraine is still going on. A lot of civilian people are dying. We need help to win this war – and I hope it will be soon.” - Daria, General Surgery Resident, Vinnytsia
“I’m going to use these skills in my operations”
“I’m a civilian anaesthesiologist in a country that is under war. I’m going to use these skills in planned operations in critical care in my emergency hospital.
Since we always have a lot of patients, with many civilians, internally displaced people, and military, who have trauma wounds, we are always lacking the materials, medication and equipment. Anything we receive (including training) we always use it.” – Igor, Anaesthetist, Vinnytsia

“I hope people are kind”
"I’m a Resident of General Surgery, trying to do all I can in my specialty. I hope I will not use this knowledge (from the David Nott Foundation training) on the battlefield, but Russia is still attacking.
I have some experience of treating war injuries. We’ve had a lot of injured people and deaths. I want to bring attention to Ukrainian refugees too who are now in other countries. I hope whoever hosts them is kind to them.” – Anastasiia, General Surgery Resident, Vinnytsia
As Ukraine continues to be ravaged by war, we have made a commitment to train every Ukrainian doctor in the country. Help us achieve our goal.
DONATE
“Maternal health - it's a societal barometer.”
Every two minutes, a woman loses her life to preventable causes related to pregnancy and childbirth. These staggering statistics stress the need for action. In humanitarian crises, where access to healthcare is severely limited, maternal care becomes even more critical.
“800 preventable maternal mortalities are happening every day, and a woman dies every two minutes from a preventable cause. So that's women dying through pregnancy and pregnancy related conditions,” shared Dr Pippa Letchworth, our Faculty Lead for Obstetrics and Gynaecology.”
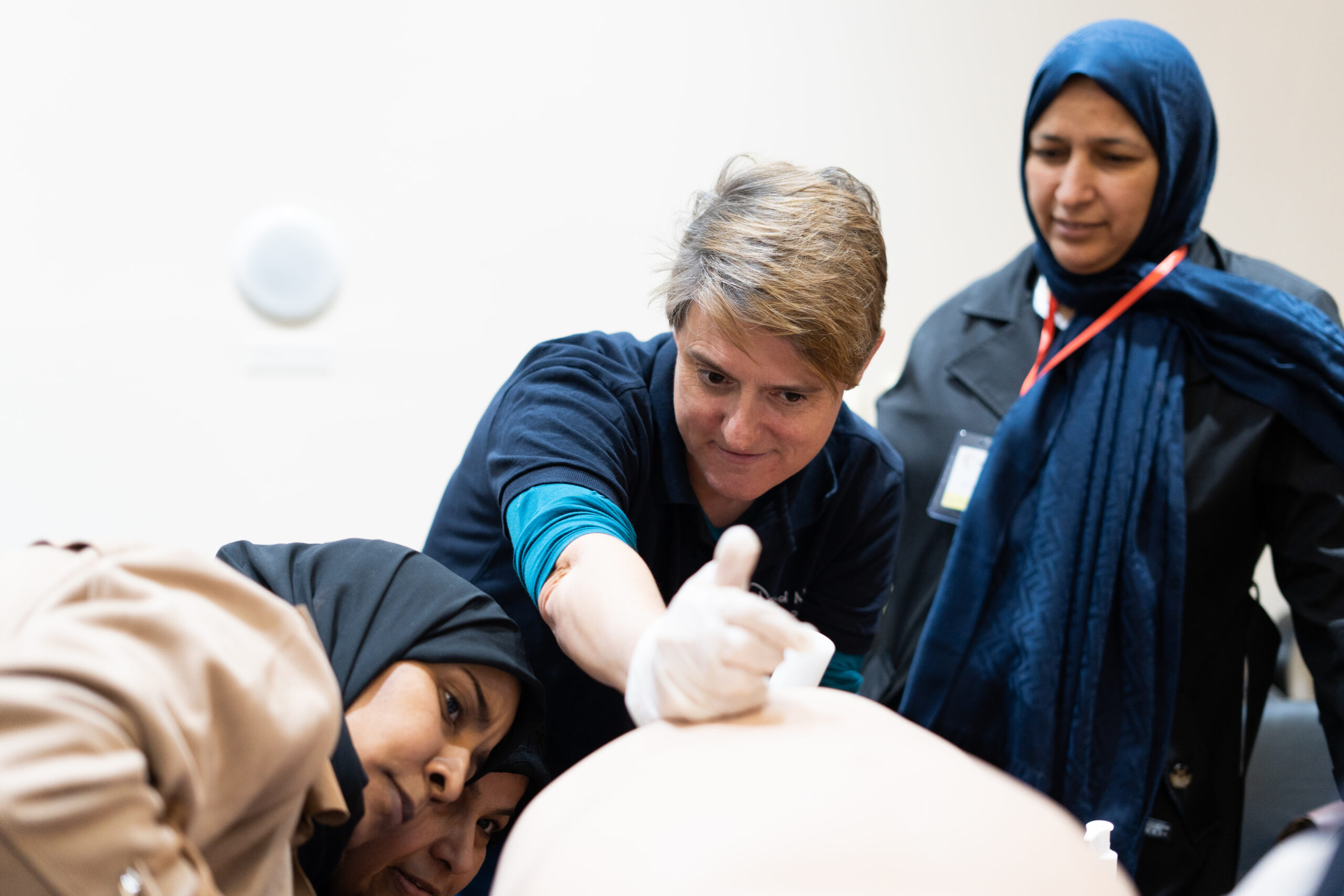
This sobering reality is what drives our passionate team to develop an obstetrics and gynaecology course aimed at addressing the most pressing challenges in maternal healthcare. In crisis settings, where resources are scarce, the course equips healthcare professionals with the skills needed to perform life-saving surgeries, particularly focusing on addressing the top global killers of women - haemorrhage, obstructed labour, sepsis, and unsafe abortion.
“75% of displaced people are women and children, and one of the five of those women will be pregnant.”
The course covers a wide spectrum of topics in maternal and neonatal healthcare in crisis. Participants begin with trauma training before transitioning into obstetrics to understand the complexities of childbirth emergencies.
Emphasis is placed on neonatal resuscitation techniques with the goal of reducing the number of stillbirths. Subsequent sessions address postpartum haemorrhage management, perineal repair, and navigating challenging deliveries like impaction and breech positions. The course also covers disruptive delivery, crucial for situations where doctors have limited access to caesarean sections.

Beyond the medical realm, our trainers advocate for a holistic approach to maternal health in their teaching. It's not just about reducing mortality rates, it's about understanding the wider implications of maternal deaths on families, communities, and societies at large. Children left motherless are at a significantly higher risk of mortality and developmental issues, perpetuating a cycle of vulnerability.
“There needs to be a call to arms to improving maternal health.”
We must advocate for women's rights, improving doctors access to education and dismantling systemic barriers that perpetuate maternal mortality.
DONATE
Our new Betty Boothroyd Scholarship Fund
We are delighted to announce the launch of our new Scholarship Fund in memory of our late Patron and beloved friend, The Rt Hon. The Baroness Boothroyd OM. The fund invites applications from medical professionals living, working or volunteering in conflict zones, including surgeons, clinicians and nurses, who wish to further their surgical training.
Our Patron
Betty became our Patron in 2016, when the conflict in Syria was at its most intense. Areas of the country were besieged, civilian infrastructure targeted and the passage of humanitarian aid restricted. Betty would often call our Co-Founders to express her concern at what was happening and ask what the Foundation could do to help.
In conflict, surgeons need a particular set of skills and decision-making strategies to be able to respond effectively to the waves of devastating injuries they encounter daily. The work of training doctors began in Misrata, Libya, moved on to Aleppo, Syria, and we have since then trained 1,825 surgeons and anaesthetists in conflict setting including Iraq, Cameroon, Palestine, Ukraine and many more.
From the very beginning of her journey with us, Betty remained deeply passionate about our training of frontline doctors working relentless hours. In honour of Betty’s commitment to our mission, we are proud to launch the Betty Boothroyd Scholarship Fund.
What’s the funding criteria?
Whether you’re a Sudanese nurse interested in a Masters in Trauma Management, a Palestinian doctor wishing to complete a paediatrics course, or a humanitarian surgeon interested in joining one of our HEST®-UK courses, we may be able to support you with funding.
Guidelines
1. Applications are open to any surgical team members who wish to further their medical training or education (e.g. surgeon, anaesthetist or surgical nurse)
2. The training that applicants are seeking funding for can be held anywhere in the world
3. Applicants must meet one of three criteria below:
- Living and/or working in a conflict or catastrophe zone
- Your country of origin is a territory that has experienced conflict or catastrophe, however you currently reside in another country
- You are a humanitarian surgeon who travels to, and volunteers in, conflict and catastrophe zones
“Thanks to Betty’s generosity to our Foundation, she will continue to make a difference to doctors striving to heal their wounded communities for decades to come.” - Elly Nott, Co-Founder
Contact us to apply
Joining forces with the Royal College of Surgeons of Edinburgh
In a landmark collaboration aimed at addressing the critical shortage of skilled surgical care in conflict and disaster zones, we are teaming up with the Royal College of Surgeons of Edinburgh (RCSEd) - home to The Faculty of Remote, Rural & Humanitarian Healthcare (FRRHH) - to deliver our Hostile Environment Surgical Training UK (HEST®-UK) course.
Taking place from 3 -7 June at RCSEd Edinburgh, the course celebrates a new era of partnership. Our HEST®-UK course offers surgeons a unique opportunity to enhance their capabilities and readiness for humanitarian crises. Over the course of five days, participants will delve into decision-making and surgical strategies for austere conditions, covering a spectrum of trauma cases including penetrating and crush injuries, orthopaedic fractures, and obstetric emergencies.
Rapid response
Responding to the escalation of the Gaza-Israel conflict in October, two previous HEST®-UK courses were swiftly organised in Bolton in December 2023 and January 2024. Obstetrician and Gynaecologist, Dr Iman Al Mabhooh, expressed his enthusiasm at the opportunity:
“I’m excited about expanding my skill set beyond obstetrics and gynaecology to acquire new abilities that will benefit mothers and their infants in Gaza and the West Bank. I recognise the desperate need for assistance there. This course is unique as it combines obstetrics and gynaecology with trauma care and address complex challenges comprehensively.”
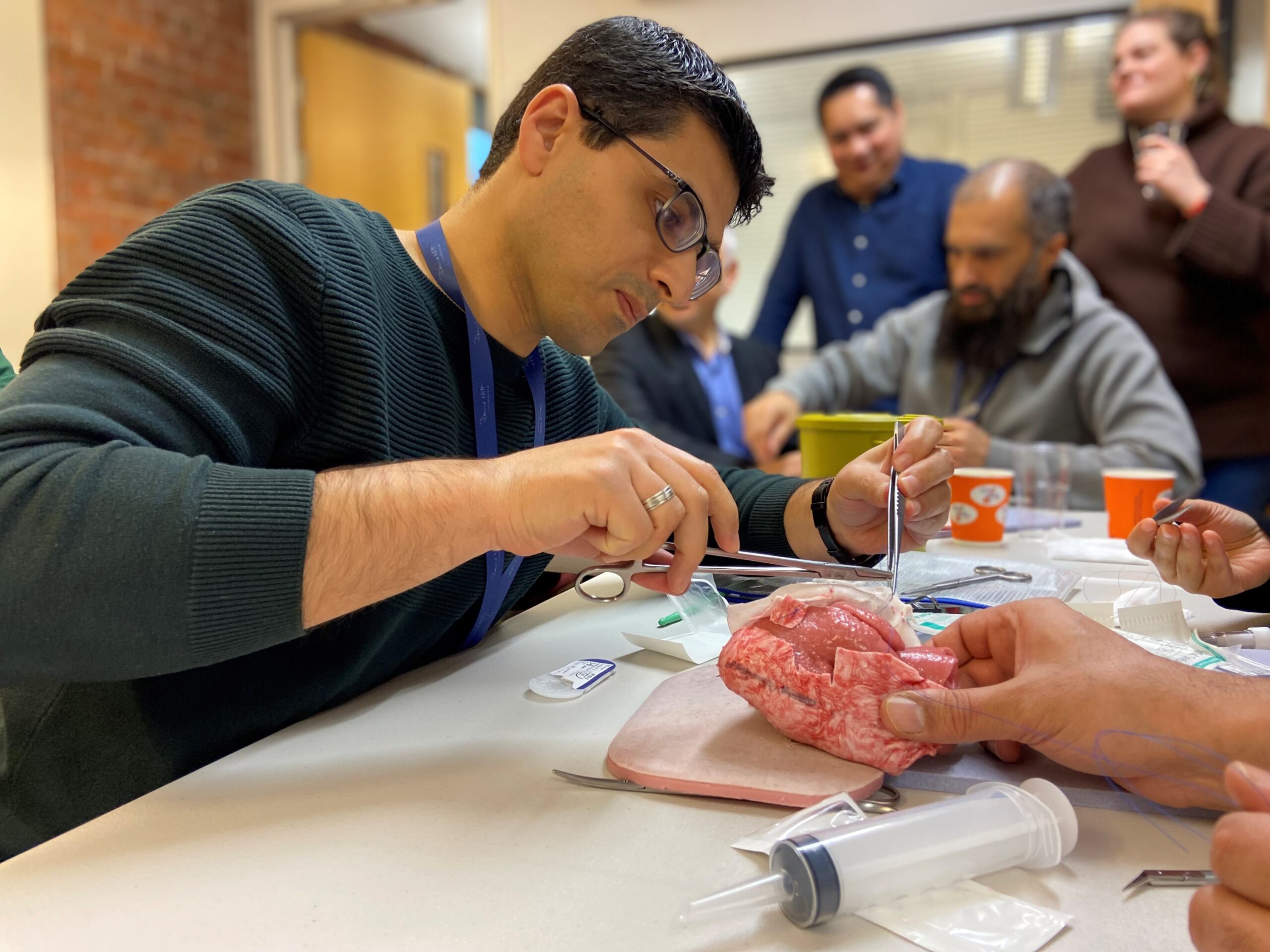
Nick Cartwright, Programmes Manager at our Foundation, said: "Since the DNF’s beginnings in 2015, our team of experienced surgical trainers have upskilled over 1800 doctors and delivered 61 courses in some of the world’s most dangerous corners, including Iraq, Syria, Yemen, Palestine and Ukraine.
With the delivery of our HEST®-UK course in partnership with RCSEd, we will grow the number of upskilled, humanitarian surgeons who are ready to volunteer their skills, make rapid and effective clinical decisions under pressure, and manage the broad range of complex trauma injuries that present in the throes of conflict and catastrophe.”
A significant step forward
Angus Watson, FRRHH Executive Committee Member, said:
“By combining the DNF's expertise with RCSEd's dedication to recognise professional standards in humanitarian healthcare, this partnership promises to empower medical professionals and save countless lives in the face of adversity.”
The Faculty's commitment to supporting surgeons is exemplified by its decision to grant participants of the course a complimentary one-year affiliation membership to the Faculty of Remote, Rural, and Humanitarian Healthcare. This membership provides an invaluable opportunity to connect with a broader humanitarian community within a professional setting tailored for humanitarian, remote, and rural healthcare professionals.
Spaces on the course are limited and will be allocated on a first come first serve basis.