“The patients. The families. They’re all in my head.”
Our Co-Founder David Nott recently travelled to Rafah, Gaza, to help treat the thousands suffering from war injuries, malnourishment, and everyday ailments that have progressed to life-threatening conditions because of delayed treatment. Here, David shares what he witnessed, what the urgent medical needs are on-the-ground, and how those he met are tattooed onto his mind.
After travelling from Cairo and getting closer to Gaza, it was quite a shocking experience. At the Rafah crossing, you could see miles worth of trucks in a queue trying to get in.
Driving through Gaza, it was like an enormous refugee camp with tents everywhere. Every single place that wasn't occupied by somebody had a tent on it. Most of the tents were so packed against each other it was difficult for people to walk.
"Thousands and thousands of people were in a small area. They had nowhere to go."
Treating those more likely to live
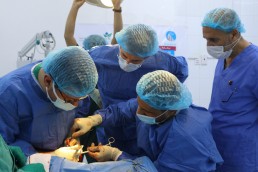
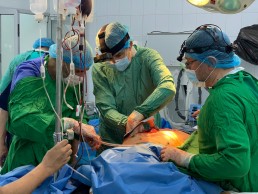
The hospital I was working in was called Al Najjar Hospital, the only semi-functioning hospital in Rafah. It was small, with a limited number of beds, but ended up housing thousands of people. Every corner was full. Patients were in the corridors, all over the wards, lying on the floor, five people where one might stand. There were people on the floor that were dying, some that had died - people crying out for help.
I had to step over people to get to patients. I had to make rapid decisions on whether or not they could be saved – decision-making techniques that we teach to those that attend our courses.
The hospital only had two operating theatres. There was no intensive care unit and no ventilators, so I had to decide which patients should be operated on with the best possible outcome. On ward rounds we reviewed those that had been treated, but many had infections because of limited sterile space or antibiotics.
18th century illnesses
"Because thousands of people have been compressed into small spaces, and many haven’t sought medical care for their everyday conditions, the clinical needs in Gaza today are astonishing."
It’s not just war wounds that doctors face – ruptured appendices, hernias, ulcers, gangrene. General surgery has been delayed for months on end and people are dying or losing limbs as a result of problems that could have been resolved quickly.
This is the reality of trauma in war – some traumas that were not traumas to begin with become life-threatening – racking up death tolls even further.
"Outside of war wounds, 21st century doctors are dealing with 18th century illnesses."
Children with chest infections were developing a condition called empyema - their infections had become so bad that their lungs were filling with pus. I’d never seen that before – it’s an 18th century condition that you would never see today.
Post-operative care felt impossible. Say you amputate somebody’s leg, there’s nowhere for them to go to recover safely. Tents aren’t sterile and it has been so cold, with the wind coming off the beach.
Calm amongst the chaos
Despite the chaos, Gazan doctors are truly outstanding. They were so warm and helpful. They were grateful that people were there to help, and together we did everything we possibly could.
This war zone is different to the others I’ve been in. The volume of people and the lack of basic medical or human resources made it incredibly challenging.
They urgently need field hospitals, more staff, a huge amount of medical resources. They need more doctors, nurses, rehabilitation services, physiotherapists. But not only that, they need a safe place for patients to go to recover after operations. Their medical aid needs are huge and doctors in the field need to be supported.
"Seeing Gaza reminds me of the vital importance of our foundation’s work. Training doctors, operating on patients in war zones, bearing witness to doctors’ needs on the ground, I’m more driven than ever to help the charity grow so we can reach even more people in need."
The patients, the families, they’re all in my head. They will always stay in my head.
SUPPORT OUR TRAINING IN PALESTINE
Bearing witness to the medical needs in Gaza
Our Medical Director Dr Ammar Darwish embarked on an operating surgical mission to Gaza to offer his trauma surgery skills to those most in need. As he crossed the border into the besieged territory, he faced trucks held up for miles, filled with much-needed aid.
“The needs in Gaza - it was hell on earth”
As Dr Darwish travelled deeper into Gaza, he observed the expanse of makeshift tents, shelters for internally displaced families. Some had no tents at all, resorting to crafting shelters from plastic sheets that offered little protection from the cold and wet weather.
Entering Khan Yunis Hospital, Dr Darwish was met with exhausted medical staff who were battling with limited supplies. Vast numbers of patients with extreme injuries came through the doors and difficult choices had to be made within minutes on who could be saved.
Adapting to an impossible environment
Lack of electricity and water are causing numerous health complications. Without electricity, patients in need of ventilation struggled to breathe. The absence of water prevented the sterilisation of medical tools. Medication, antibiotics, painkillers, and even anaesthesia were sparse – basic resources that should be present in any hospital.
Children with severe injuries from shrapnel lay in beds with little to no relief due to lack of medical resources.
“I met a very scared six-year-old boy that had a shrapnel injury in his abdomen. Because of the complexity of the injury, and because of limited resources such as antibiotics, the boy’s abdomen was open and there were a lot of holes in his bowels. Anything he ate or drank was leaking out of his abdomen. That child had not had any food to eat, or a proper drink, for a whole month, he was a skeleton.”
Stretched to limits
Despite the chaos, resilience and humanity ran through the Gazan people. Local medical staff welcomed Dr Darwish and his team, despite managing the loss or unknown status of their homes or family members. They were stretched to their limits, with only nine operating hospitals left of all the 36 hospitals in Gaza.
“You cannot but compare it to our work in a UK major trauma centre, where for one trauma patient, you might have six, seven, even 10 doctors treating them. In Gaza you are one doctor for 10 people, 15 people, which means you have to make really heavy decisions on who to treat. It sits heavy on my heart that there were many children we could not even see to in time.
I've been part of over 45 global missions in conflict zones, with Syria, Aleppo, being one of the most challenging. This mission to Gaza was the most difficult mission that I've been through physically, mentally, even psychologically, because of the amount of injury that I witnessed and the amount of devastation and carnage we were faced with and with only basic supplies and resources.”
Medical needs for years to come
“The number of injured people now in Gaza has exceeded 70,000. If you can imagine the complexity of these injuries - these patients will need years of medical care, surgical operations, physiotherapy, and a lot of resources to reconstruct their injuries. There is a huge need for humanitarian aid, but first there must be a ceasefire.”
We have provided training to 79 UK surgeons who are preparing to or have already travelled to Gaza to provide life-saving aid. Many more are scheduled to depart. Our aim remains steadfast and unwavering – to ensure everyone has access to safe, skilled surgical care.
We are committed to supporting the Palestinian people until we are able to train in-country again.
SUPPORT OUR TRAINING IN PALESTINE
41 Syrian doctors upskilled to screen and treat women with cervical cancer
Dr Saladin Sawan, Consultant Surgeon in Gynaecological Oncology and one of our faculty trainers, recently returned from a surgical mission in Idlib, Syria, upskilling 41 surgical residents and specialists to screen for and treat women with cervical cancer. Here, Dr Sawan shares his hopes for healthcare and future training in northwest Syria.
Syria remains engulfed in a complex humanitarian crisis. Over a decade of conflict has forced more than 12 million people to flee their homes and left displaced communities with reduced access to food, shelter and protection.
Cancer under the radar
Due to a buckling healthcare system and greater focus on other urgent needs, many are not seeking or receiving the cancer screening, diagnosis or treatments they need. Medical professionals also face challenges with transferring patients over the border to Turkey, which means cancer patient numbers in-country are growing.
Cervical cancer is preventable and curable, as long as it is detected early and managed effectively. According to the World Health Organisation (WHO), it is the 4th most common form of cancer among women worldwide.
Our faculty trainer, Dr Saladin Sawan, travelled to Idlib to upskill Syrian surgeons to offer the best possible surgical care for patients with gynaecological cancers including cervical cancer.
“During my mission, I delivered gynaecology training to a group of doctors. Every day, we practiced surgical techniques. We used chicken thighs and a cutting-edge mannequin, provided by the David Nott Foundation, to practice performing cervical smears, colposcopies to assess the cervix for cancer or pre-cancer changes, and diagnostic punch biopsy, in addition to safely performing treatments for pre-cancer cell changes, in the form of loop excision (using heat to remove cells). Each doctor had hands-on practice and then we put skills to the test in operations.”
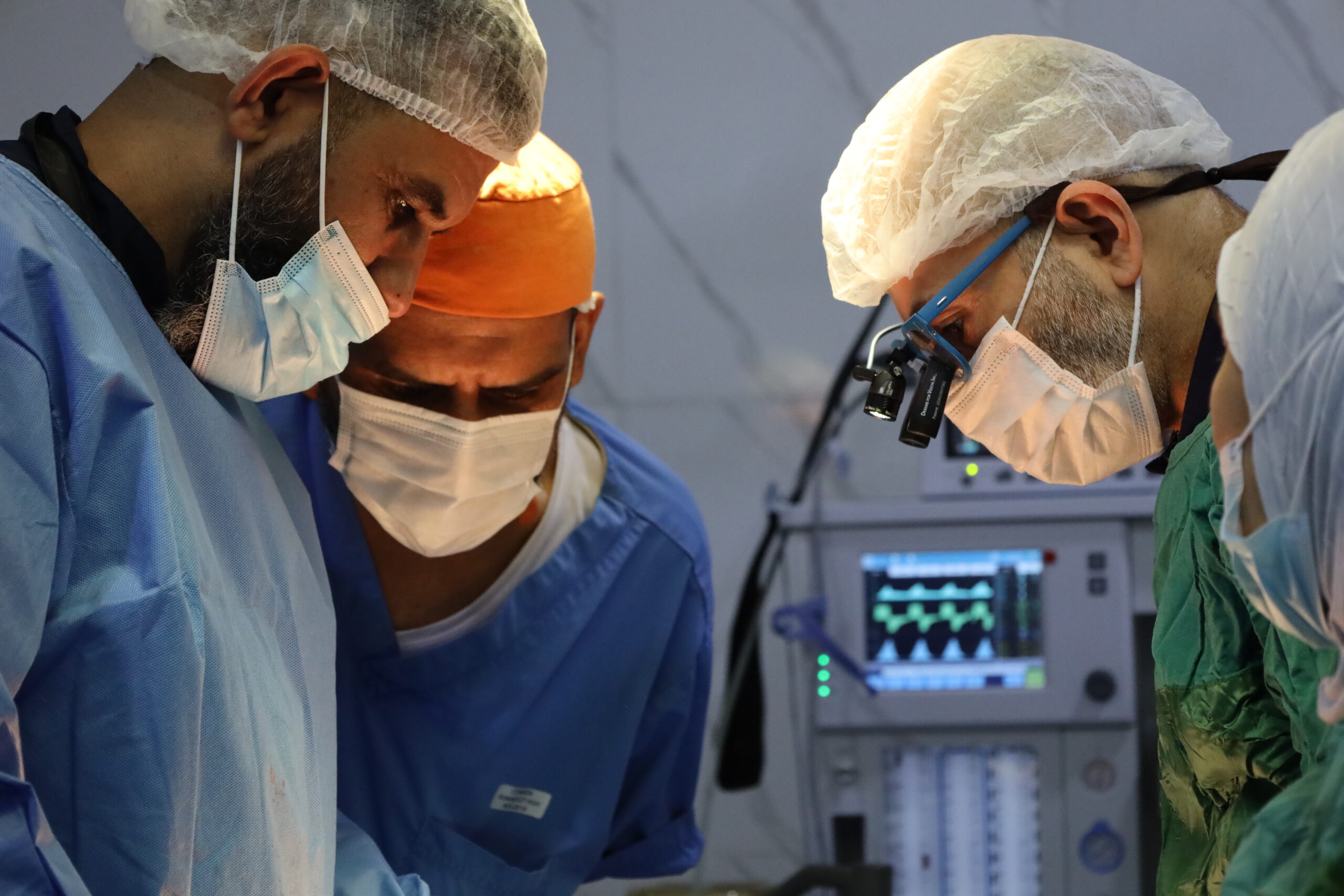
Dr Sawan trained 41 local doctors during the mission, which will improve cancer patient care while strengthening northwest Syria’s healthcare system in the long-term.
“I performed approximately 14 surgeries of different magnitude, some small procedures, some far more complex, for example radical hysterectomies for cervical cancer patients and debulking surgery for women with ovarian cancer. We used operations as teaching opportunities for local doctors – residents were assisting me and watching over my shoulder. We trained anywhere between three and seven obstetrics and gynaecology residents per day. Some doctors followed me, but I made it my goal to visit as many hospitals as I could to deliver training to those who could not travel. I was very happy.
I felt appreciated amongst a family of doctors and health professionals who looked after each other to deliver the best they could for their patients in some of the most difficult circumstances. I was certainly privileged to have had the chance to be with them.”
Eliminating cervical cancer
Due to ongoing conflict and accessibility issues, doctors in northwest Syria have limited access to training. The province also lacks a screening programme for cervical cancer prevention and early detection, leading to increased numbers of cases that require complex, radical surgery.
“WHO launched an Elimination of Cervical Cancer Elimination Initiative, which mainly targets low-income countries. The local doctors are really excited about establishing this program for women in Syria. They know the benefit, they believe in its value and importantly they feel it is only right to do since women disproportionately suffer the results of human papilloma virus infection which causes cervical cancer, unlike men. This would promote healthcare equity.”
In his training, Dr Sawan actively encouraged the local doctors not to fear making mistakes.
“Doctors become more confident and patients as a result will be safer. We strive for the doctors to test, try, play, make mistakes. The intention is that the doctors are more competent by the time they perform the operation on patients.
I am lucky to be part of the David Nott Foundation where the emphasis is also on building local expertise and sustainable care by training local health professionals in crisis areas. The donated equipment and surgical instruments meant I was able to deliver comprehensive training without compromises.”
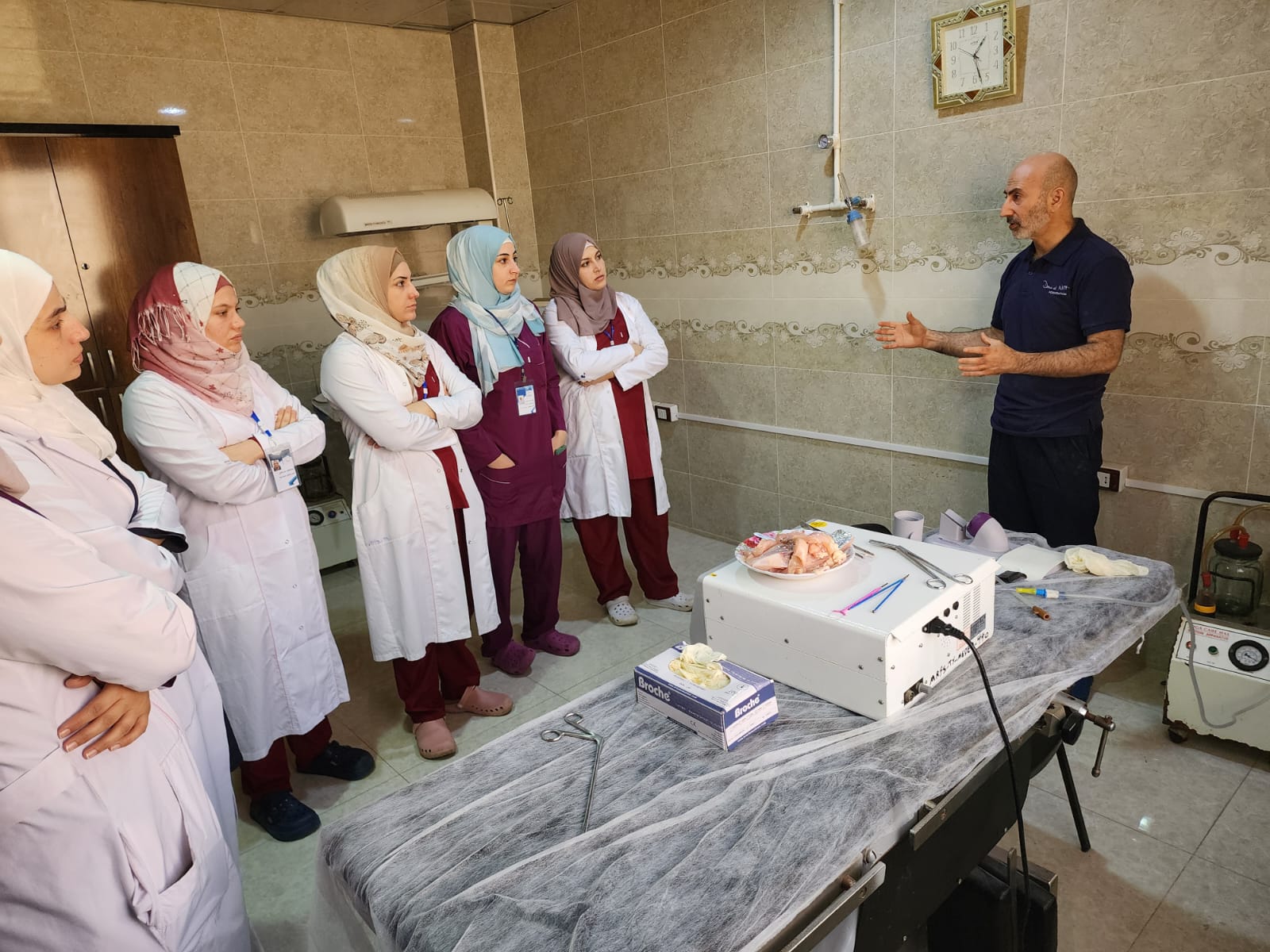
Glimmers of peace
“Around me in Idlib, despite being in a region struck by war, there were people trying to rebuild their lives. Developing roads, restaurants opening, people moving into the city. People have started to live their lives – the dust of war settling and communities trying to get their lives back.”
Since Dr Sawan’s mission and apparent signs of a healing community, the Regime has targeted 45 cities and towns in four days, killing 52 and injuring over 240, according to an October recent report led by Assistance Coordination and Information Management Units (ACU, UMI). Despite glimmers of hope, northwest Syria remains in the thralls of conflict.
What’s next?
As unrest continues, the need for training and sharing of knowledge remains. We are committed to upskilling even more obstetric and paediatric residents in northwest Syria, but there’s much more to do.
“Outside of returning to deliver more surgical training, we also want to deliver dedicated cervical cancer screening training to residents,” shares Dr Sawan.
On-the-ground partners have also identified other, urgent areas of need.
“A local humanitarian organisation, the White Helmets, are looking to develop training for paramedics, including resuscitation and emergency obstetrics, gynaecology and neonate training. To make sure we provide the right training material for paramedics, we want to speak to them to understand exactly what their needs are in the field.”
We’ll continue to do all we can to support medical professionals in Syria.
“The need in Syria is astonishing”
We’ve just returned from northwest Syria after training 23 local doctors to surgically treat complex wounds caused by the earthquake that shattered parts of Syria and Türkiye in February. Our CEO, Elly Nott, shares her reflections of our latest mission and how we will continue to stand with Syria.
As soon as we crossed the border into Syria, fields of olive trees stretched as far my eyes could see. Row after row, the trees continued until we reached Atmeh.
Our destination was Aqrabat Hospital, where I was leading a surgical mission to train local doctors to provide specialist orthopaedic and plastic surgical care to the survivors of February’s devastating earthquake.
The need for our training is astonishing.
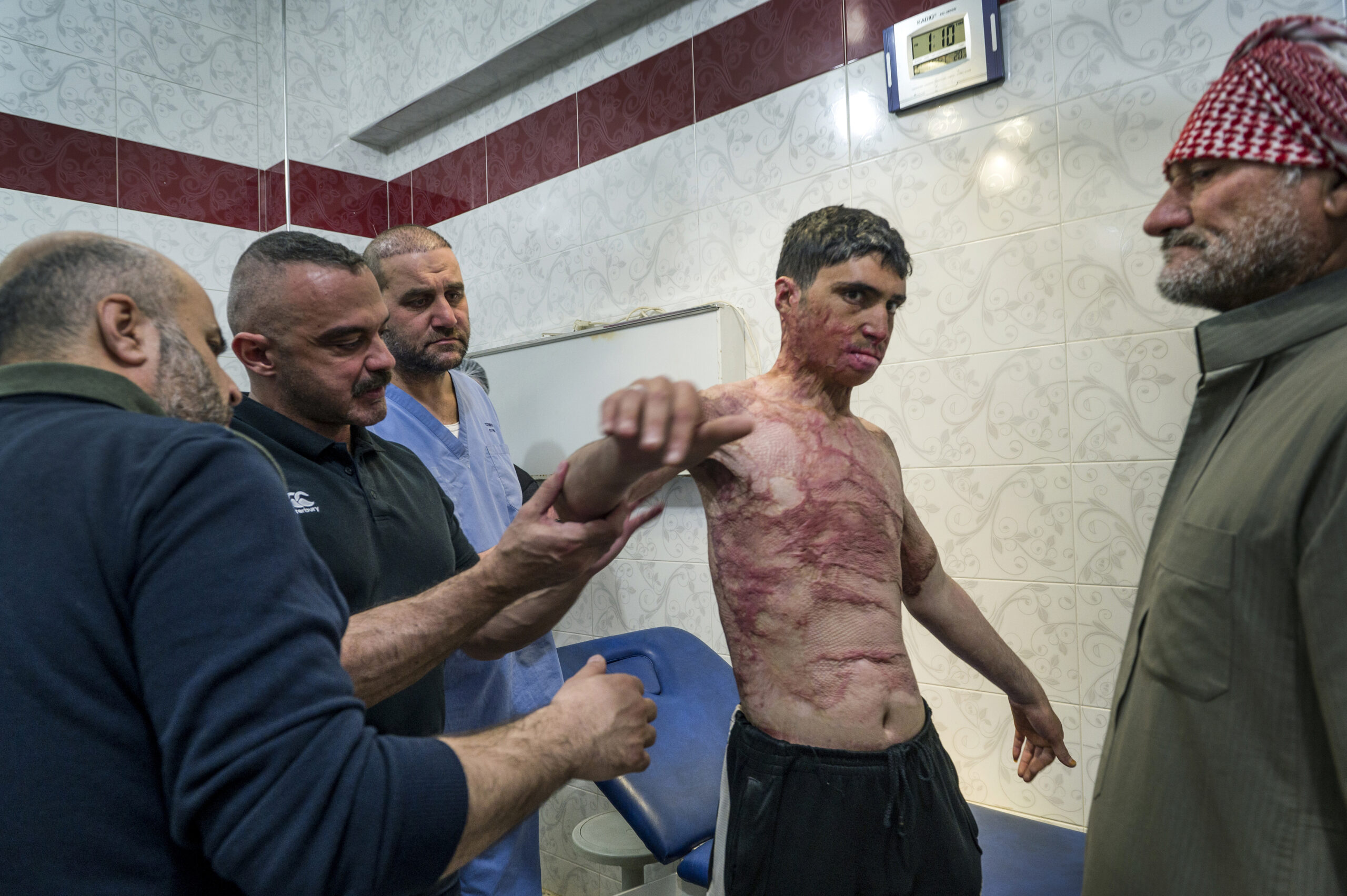
After hearing that ours and Action for Humanity’s specialist doctors were visiting, a staggering 2,000 people sought care at the Hospital.
Action for Humanity’s team, who led the operating arm of our mission, saw 300 in clinic and were able to surgically treat over 60 patients over a week period. At the same time, in rooms above the operating theatres, we taught 23 Syrian doctors with the skills needed to treat complex trauma injuries inflicted by earthquakes or the ongoing conflict. Our team also taught nine Syrian surgeons to become David Nott Foundation trainers themselves, leaving a lasting legacy of shared knowledge and confident doctors in Syria.

Aqrabat sits in northwest Syria and is supported by a remarkable network of civil society organisations and NGOs. Despite this, the region is vulnerable. The hospital serves a population of around four million, the majority of whom are dependent on humanitarian aid. Some 2.6 million of residents have already been forcibly and repeatedly displaced from their homes by the conflict from places including Ghouta, Dara’a, Homs, Aleppo. Families faced food and fuel shortages and health challenges including a cholera outbreak. The recent earthquakes have added further pressure to weakened economies and healthcare systems across the country.
As conflict and the effects of the earthquake continue to fuel instability, we must not abandon Syria.
Speaking to doctors we’ve trained, it’s clear our mission has had a lasting impact. Many have commented on their restored confidence and others that they now feel better equipped to treat those most in need.
A personal highlight for me was meeting Syrian doctors who had learned from, met or heard about my husband and Co-Founder, David Nott. Many had operated alongside David in underground hospitals in Aleppo while the Assad Regime and its Russian allies bombed the east of the city relentlessly in 2013 and 2014. Their connection with David, despite the passing of years, reinforces just how powerful shared knowledge is.

Our Faculty Director for this mission, Dr Ammar Darwish (pictured below), who is originally from Syria, shared:
‘Going back to Syria was one of the happiest days of my life. Crossing the border and seeing Syria again, with all the sadness and monstrosities that have happened, there’s still a sense of happiness, a sense of pride. It was a very special feeling. Training the doctors there and seeing those we’ve worked with and taught before was something else. It put tears into our eyes.’

Northwest Syria faces vast challenges. We cannot remedy a decade of pain, but we can continue to arm surgeons with life-saving skills and show them that we stand beside them.
We’ll be back to train more doctors soon.
Elly Nott, Co-Founder and CEO at the David Nott Foundation
“One day, change will happen. Until then, we’ll keep the flag flying”
On Friday 21st October, David was interviewed by the Chair of Action for Humanity, Dr Ayman Jundi, at the University of Central Lancashire (UCLan). He shared stories from the frontline, the bonds he formed in Syria’s underground hospitals, and how he copes with the monstrosities of conflict.
We were delighted to be joined by over 200 attendees, consisting of supporters, medical students and UCLan staff members. All listened intently as David offered a personal insight into his work and mind.
Becoming a war doctor
“Back in 1993, I’d just become a consultant surgeon at Charing Cross,” shared David. “I was watching the news about the Bosnian war and the terror going on there. Similar to Ukraine, Sarajevo at that time was being shelled heavily. I remember the story of a man looking for his daughter. He found her, pulled her out the rubble and took her to hospital, but there was no doctor there.
That’s when I thought, I have to do something.
The following morning, I couldn’t wait for the sun to come up. I called Médecins Sans Frontières (MSF) and two days later I was in Sarajevo.”
David’s experience in Bosnia - performing difficult surgeries on injured civilians in the freezing cold – lit a fire in him and he was soon grabbing every opportunity he could to take unpaid leave and travel to where he was needed. In 2012, David’s work in Syria began.
The first Syrian mission
“I was in Libya with MSF. It was then that I got a call about a conflict in Syria. I first travelled to Atmeh in Northern Syria, which was very dangerous. The medical set-up was not good.”
There were few ambulances in the region, so cars and vans were used to transport the injured to make-shift hospitals. They’d screech to the entrance and beep their horns to alert doctors inside.
“The hospital we worked in at that time was a converted house. The dining room was the operating theatre, the kitchen - A and E, and bedrooms were turned into wards.
At the beginning of the conflict, there were incidents of people making bombs in their homes. Unfortunately, there were many accidents, leading to awful blast injuries and loss of limbs.”
Action for Humanity
Following Atmeh, David began working with Action for Humanity (formerly Syria Relief) to lead multiple surgical missions in Syria.
“Starting my work with Syria Relief, now Action for Humanity, was the best thing I’ve ever done. They helped me enter the heart of Aleppo, which will always stay with me.
In Aleppo, I was predominantly teaching, so skills were left with the doctors living there. I did some operations to show them how to do things, but after they learned a procedure, I would assist and help. They knew what to do.”
“I was determined to get them out”
Working shoulder to shoulder with Syrian doctors naturally led to strong friendships built on the foundation of shared humanity. In 2016, bunker-busting bombs were destroying buildings and obliterating underground hospitals in Aleppo.
“I thought everyone I’d come to know, all of the doctors I’d met, were going to get killed. I was determined to get them out.”
David contacted President Assad’s office and after four days of trying, his call was connected and he made his case with passion. David will never know if his efforts contributed to the ceasefire that later followed, but he was elated when his friends were granted safe exit from eastern Aleppo.
“There were so many wonderful people working incredibly hard to get a ceasefire. I hope I was able to play a small part.”
Coping with conflict
When asked during a very engaged Q and A how he copes working in conflict zones, David shared:
“You have to be resilient. It can’t be taught to be honest - it’s learned with life experience. There are some things that are out of your control though – the terror that someone might come for you.
After Aleppo, I needed treatment, which helped. But if it’s terror during work or a patient case, talk about it, share the load, you’ll get through the hard times and become more resilient over time.”

A Masters of Disaster Medicine student at UCLan asked, ‘What can we do about healthcare systems being targeted in conflict?’
“Healthcare is indeed used as a weapon of war,” said David. “It’s like a form of psychological warfare. The act of killing a doctor takes down the psychology of whole communities.
We’ve stood on podiums and talked about how we need to protect doctors, written a letter to the Prime Minister, raised placards on a protest in London. We’ve got to do what we can to support healthcare workers.
One day, change will happen. Until then we’ll keep going, we’ll keep the flag flying.”
Meeting Heston®
The event ended with a reception, giving guests a chance to meet our team and our one-of-a-kind surgical simulator model, Heston®, beautifully presented by Manchester’s Friends of David Nott Foundation (FDNF) Society.
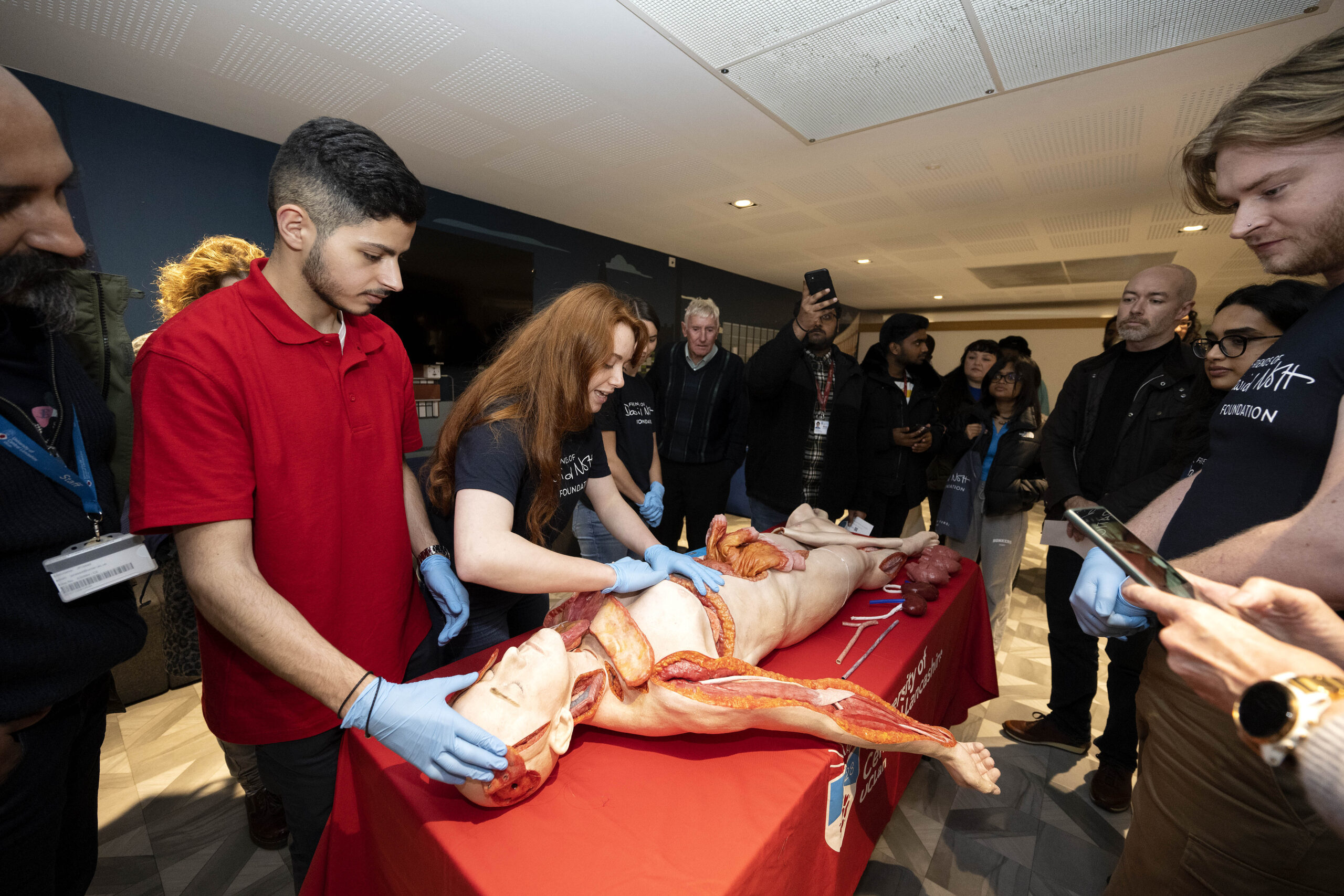
Dr Ayman Jundi, Chair of Action for Humanity and Clinical Senior Lecturer and Disaster Medicine Course Leader at the University of Central Lancashire, said:
“I was honoured and privileged to have a conversation with David Nott. His honest, down-to-earth and inspiring approach engaged the audience and instigated a wonderful and fulfilling discussion.”
"The skin is alive - it's all because of you."
“Here – you do it.” These were the words of our Co-Founder David, as he handed a skin grafting instrument to Ivan, a junior doctor in eastern Ukraine attending our surgical training course.
During a Russian shelling, a woman suffered catastrophic leg injuries. Working to repair her wound during a mission in Ukraine, David used the surgery as an opportunity to train local doctors.
He showed them how to perform a skin graft to treat the injury – and that wrapping the graft in fluffy gauze can help with healing. This technique differs to standard wound treatment, which often involves the application of antiseptic spirits and bandages.
David and Ivan have kept in touch since his returned to the UK – a common story for David and our trainers. We are proud to have created a supportive community of war doctors that can ask questions or share cases with us at any time, from anywhere.
When Ivan looked at his patient’s wound in recovery, he was overwhelmed with joy to see that it was healing. During a phone call, he shared with David:
“The skin is alive! It’s all because of you.
I’ve started a little revolution in my hospital. I’ve started to do what you do - using the fluffy gauze for skin grafts. The patient’s granulation (tissue that is an important component of wound healing) is awesome. We haven’t needed to use any antibiotics.
It was one of the best moments of my life doing this operation. I can only say thank you for your knowledge.”
Ivan, a junior doctor facing the horrors of his country’s war, is now armed with a skill that can be used to treat devastating injuries. He plans to teach this technique to his peers – and potentially even senior doctors who typically use other methods.
Although unusual for a junior doctor to teach senior consultants, in war, titles are stripped away. All that matters is the sharing of knowledge and saving of lives.
To carry out the next phase of the patient’s skin graft surgery, David offered his help over Skype. Ivan and his father, a Chief of Surgery based in Kharkiv, will work together with David to rebuild the woman’s leg and remove as many traces of the evidence of war as possible.
Surgery over Skype isn’t new to our Co-Founder. During the historic siege in Aleppo, David guided surgeons online as they reconstructed a man’s shattered jaw. The Syrian surgeons, Dr Assaf and Dr Baydak, successfully carried out the operation and put the man’s face back together again.
The stark similarities between Syrian and Ukrainian conflict do not go unnoticed. As witnessed in Aleppo, healthcare workers in Ukraine are in urgent need of our support. As the war continues to wage on, we are more driven than ever to train doctors and help them prevent needless deaths.
“You have given me new breath in surgery,” shared Ivan. “You were not scared to come here and share knowledge. Thank you.”
More on our training in Ukraine
Mosul to Manchester: Our war surgery training in practice
Dr Moez Zeiton is one of our surgical trainers. As a humanitarian surgeon, Moez has witnessed the realities of war, but never expected to see similar horrors on British ground. Here, Moez shares his journey to joining our teaching faculty and how he’s used his surgical skills around the world.
Moez’s first exposure to medicine was through his father training as a general surgeon and specialising in oncoplastic breast surgery.
“I sort of drifted into medicine myself. I loved biology at school, but my love for the sciences and in particular, my inspirational high school Biology teacher shaped my decision to study it. When I started the course at the University of Leeds, I remember loving the anatomy and dissection work and knew surgery and acute trauma were fields I was interested in,” Moez shares.
A fork in the road

“My entry into humanitarian work started by accident. I always felt a connection to the Middle East through my family and having regularly travelled there as a child to visit extended family and friends.
So, when the Arab Spring uprisings in 2011 arose, I got involved with charitable initiatives sending medical aid and worked on advocacy, opinion pieces and articles. I knew I wanted to be there on the ground, so I negotiated a one-year sabbatical from my surgical training. At the age of 25, I left for Libya to do my part.”
Moez worked with non-government organisations and local Libyan doctors, opening him up to the world of humanitarian health. This led to him taking on a voluntary role as National NGO Coordinator for six months. He also attended courses on analysing disrupted health systems with the World Health Organisation (WHO).
Taking part in our training
After his sabbatical, Moez continued his surgical training in the UK and fed his interest in humanitarian surgery with research. He was part of The Lancet’s series on health in the Arab world and commission on global cancer surgery. He also attended the Scholars in Health and Research Programme at the American University of Beirut.
Working at a major trauma centre in the UK, Moez worked alongside some of our senior faculty and was introduced to our Surgical Training in Austere Environment (STAE) course. He was one of the first doctors to benefit from our scholarship programme, attending our STAE course in 2017.
“On the final day of the course at the Royal College of Surgeons, I met people from WHO and Aspen Medical International who were looking for doctors to help with trauma victims in Mosul, Iraq, following ISIS invasion. Two months later, I found myself there, with a group of expat and Iraqi doctors.
Immediately, I was able to put my new war surgery knowledge to practice - damage control and how to save lives and limbs.”
War wounds in Manchester
Two weeks after returning from Mosul, Moez was unexpectedly faced with war injuries in Manchester – blast wounds following the Manchester Arena bombings.
“The injuries I saw were very similar to what I’d seen in Iraq and had been teaching on the Foundation’s courses - blast injuries from shrapnel and metalwork. I was able to use what I’d learnt but now in my home country.
Although it was shocking and very stressful, things worked seamlessly in our hospital and the camaraderie, hard work and collaboration I saw across 7 or 8 local hospitals that received injured patients was unlike anything I had seen before. I truly saw the NHS at its best.”
Becoming a trainer
“After my return from Mosul, I was invited to join the Foundation’s orthopaedic faculty. Being part of the Foundation’s faculty for the past 5 years, teaching the skills I learned on that STAE course in 2017, is incredibly special.”
For the first time, Moez led the orthopaedic section of our recent course in Gaziantep.

“Although I had been teaching on the STAE course in London for some time, the oversea HEST® course required a slightly different approach. I needed to prepare and familiarise myself with the course material. Attending the Train the Trainers course which was put on by the Foundation really helped with this.
The 26 Syrian surgeons we trained shared incredible stories and the cases they faced during conflict with limited resources. Rather than teaching, I facilitated discussions around patient cases, learning from shared experiences and taking things back to fundamental principles. I learned just as much from the inspiring candidates as they learned from me!
This was also the first time that I had delivered an all-day comprehensive professional course in Arabic. It was extremely challenging considering I’ve only practiced medicine in English. However, the feedback and appreciation that I received from attendees is certainly one of the best achievements in my career.”
Leaving a legacy
Looking to the future, Moez wants to continue serving those in need in the UK and around the globe.
“I feel passionately about my humanitarian work and want to continue this in tandem with my NHS role, ideally doing one or two missions a year.
The NHS is such a huge organisation and has a vast resource of skills, knowledge and cultural experiences that can be tapped into. The world is incredibly connected. No matter how far away they may seem, conflict and disasters that happen in other countries continue to affect us directly or indirectly through human migration, security and the economy. We should be using our training and unique cultural experiences to help others around the world.”
Help us train more war doctors
David reflects on his latest mission in Ukraine
Our Co-Founder David Nott recently travelled to Ukraine with UOSSM International, performing life-changing surgeries and offering guidance to doctors across the country. Here, David shares his reflections on what will remain a memorable and emotional mission.
My latest mission to Ukraine was an incredibly important one for me. I travelled everywhere, north, south, east and west.
I initially started in one hospital. When they knew what I could do, I was asked to go to more hospitals, and it started to snowball from there. I began by treating a number of old war injuries, people that had holes in their legs and arms, loss of shoulders and big fragmentation wounds.
It was clear that Ukrainian surgeons wanted support with plastic surgery. Many didn’t know how to rotate flaps, some had never seen one before. Many had never done war surgery at all. So, I spent my first week just operating and operating - doing all I could.
At one point, I had 14 or 15 people in an operating theatre all bent over watching what I was doing. It's a great way to teach - I stood back and told them where to make the incisions. They were delighted to learn.
I reconstructed a patient’s shoulder that had been blown off and other serious blast wounds. When I went back the next day to see one of the blast patients, they gave me a thank you plaque which was incredibly kind. They were desperate to have somebody show them what to do – someone there to help them.
I travelled all over the country to regions that have now been heavily bombed. I saw how refugees in Lviv are gathering in a railway station, and the fantastic work that NGOs are doing there. There are thousands of people, all being fed and sheltered with the help of outstanding charities.
Now having seen the devastation, it feels like the exact same tactics as in Syria. When I was in Aleppo in 2016, the whole region was completely and utterly destroyed. What we’re seeing in cities like Mariupol – the destruction - feels very similar to what I witnessed in Aleppo.
Teaching has carried on here in the UK. I taught a doctor called Oleksandr who contacted me when I was back home. He watched me repair a serious leg wound in Ukraine and had seen the condensed training videos we made for surgeons there, but Oleksandr was now the lead surgeon faced with a similar blast injury.
I guided him through his surgery remotely, as he took a flap of skin from behind the knee to repair and close the wound.
"I was quite nervous, but it went well thanks to David Nott. He showed us ordinary doctors how to fight on the medical frontline." - Oleksandr
Oleksandr and his colleagues are treating awful injuries that no-one should ever experience. But the injuries will keep coming, so it’s my hope that they will pass on what they’ve learned. By sharing my knowledge and 30 years of war surgery experience, a lasting legacy is created.
There’s a huge amount of work to do. I think surgeons and healthcare professionals in Ukraine will be faced with war wound reconstructions for many years. Plastic surgery will be incredibly important as the conflict continues – and far into the future too. The Foundation will do all we can to help doctors navigate this war and its aftermath.
Operating and Teaching in Yemen: an Interview with David Nott
In April, David travelled to Yemen with Ammar Darwish, Mounir Hakimi and Asan Raffee to deliver both teaching and hands-on surgery in the World's worst humanitarian crisis. Below is a short interview that we conducted with him on his return.
How did this trip come together?
It came about with a telephone call from Syria Relief. Mounir Hakimi (of Syria Relief) had been in contact with several of the doctors who had been working in Marib. They were operating on a large amount of cases and they wanted help. Some of the surgeons who were there had difficult wounds or injuries presenting, and they wanted advice and teaching on how to cope with those injuries. That was how we heard about it.

The Syria Relief - DNF Team break their fast in Marib.
What did you see of the city of Marib?
It was pitch black at night when we arrived. We landed in Seiyun and it was a 6 or 7 hour drive to Marib. We arrived very early in the morning and went to a hotel local to the hospital. A few hours later, in the morning, we went to the hospital and were very much welcomed by the medical team working there.
What was the hospital like?
We had a very nice tour around. The Medical Director was extremely enthusiastic in showing us exactly what they had been able to continue to do. They had a very good blood transfusion bank, they had very good blood chemical laboratories. They had an intensive care unit, they had well-stocked theatres and they had a good array of back-up support. There were a lot of nurses on the wards.

At the time, Marib was becoming the epicentre of the civil war. Could you see that that hospital and its staff had been affected by escalating conflict within and around the City?
Yes. It was the epicentre. And it still is. The fighting is intense. Probably about 15km north of Marib. At the moment, Marib has about two million refugees and it is very densely populated. The fighting is continuing and obviously the hospital that we were in was the frontline hospital to accept all those casualties that were wounded. Both civilian and non-civilian.
We heard jets going over the top and we also heard rockets coming into Marib. You were aware that you were in a very hot war zone.
Who did you meet at the hospital?
Some were senior doctors. Some had just come in the last couple of months from Egypt to help out. There were quite junior doctors. There were those that required quite a lot of teaching and understanding of how to manage injuries. The hospital had stopped almost all of its elective surgeries. They were focusing purely on the war-wounded patients. Unfortunately those patients that had cancer problems weren’t really dealt with at this time.
Which case stands out the most in your memory?
I think the case that stood out most was after the teaching we gave the night before on gunshot wounds to the chest and abdomen. The surgeons had never done a thoracotomy before for a gunshot wound to the chest. The following night we were called back to the hospital with a surgeon who had watched our lecture and we found there was a patient who needed a thoracotomy. Because we were there, we were able to show him exactly how to do it and exactly how to extend this incision onto the abdomen and do a thoracoabdominal procedure. The patient did extremely well and thanked us a couple of days later.
We discussed a lot of reconstructive work. Most of the flaps that we discuss on our HEST® course, we did in Marib. There was a lot of surgery done with a view to the surgeons being able to do that kind of surgery when we left.
Going forward, what do you think the Foundation's work in Yemen is going to look like?
I think that we will be going back to Marib, and I think we will continue to go back and support them both with teaching the DNF HEST® course and perhaps this time taking our models with us as well so that we can run a course during the day or the evening and then operate as well. I think the future of the DNF is operating as well as hands-on teaching as well as the classroom for some courses. The future lies both within the operating theatre and the classroom.
I think we had developed a significant rapport with the doctors such that I heard recently that they desperately want us to go back again to show them more and more. I think that is the perfect opportunity for the DNF to show what it is worth really.
This mission epitomised what the DNF is all about. The DNF goes out to the field, it saves lots of lives as well as teaching the doctors so that they can continue to save lives. The DNF leaves a legacy.
You can read Ammar Darwish's story of the mission here.